Can anesthetic and analgesia treatments affect cancer recurrence and metastasis? - Part 5
Posted by Doctor Nguyen Thi Hoai Nam - Department of Surgical Anesthesia, Vinmec Central Park International Hospital
Effects of co-transfusion; Effects of psychological stress; The effect of perioperative hypothermia on cancer recurrence as well as retrospective clinical evidence on the association between regional anesthesia and cancer recurrence will be discussed in the text.
1. Effects of co-transfusion
Allogeneic transfusion is associated with immune regulation and may also be associated with an increased risk of cancer recurrence, infection, and perioperative mortality. Transfected leukocytes may be involved in transfusion-associated immune regulation, resulting in changes in circulating lymphocytes, helper T cells, suppressor T cell ratios, and B cell function . Irradiated or leukocyte-depleted red blood cells are commonly transfused in cancer patients, an association has been observed between patients transfused with leukocyte-depleted red blood cells and a significant reduction in survival. disease and overall survival compared with patients who did not receive a blood transfusion. A recent meta-analysis examined the effect of blood transfusion on cancer recurrence, disease-free survival, and overall survival in patients undergoing resection for lung cancer in 5378 patients. No firm conclusions can be reached, however, there seems to be a link between blood transfusion and reduced disease-free survival.
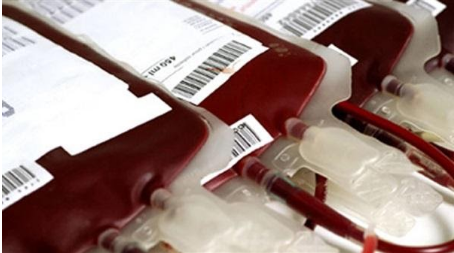
Truyền máu đồng nhóm có thể làm tăng nguy cơ tái phát ung thư
2. Effects of psychological stress on cancer recurrence
Up to 30% of women with breast cancer experience anxiety and depression, and a history of depression can predict cancer recurrence and overall survival. Psychological stress and perioperative anxiety stimulate physiological stress responses through the hypothalamic-pituitary-adrenal axis and the sympathetic nervous system. This leads to the release of glucocorticoids, endogenous opioids and catecholamines that have a significant impact on the tumor microenvironment. It is thought that β-adrenoreceptor antagonists may inhibit some of the deleterious effects of stress.
Women taking propranolol, a nonselective β-antagonist, during the 1 year prior to breast cancer diagnosis were less likely to have local tumor invasion and had a lower cancer-related mortality rate than women Females do not take propranolol. This effect was not seen in patients receiving the selective β1-antagonist atenolol, but the small number of women in the propranolol cohort and retrospective data suggest that this result should be interpreted with caution.
3. Effect of perioperative hypothermia on cancer recurrence
Up to 70% of anesthetized patients experience unintentional perioperative hypothermia due to the cool operating room temperature, hypothermia due to anesthesia, and convection air in the operating room. Hypothermia causes changes at the cellular level that negatively impact innate and adaptive immunity. The incubation period of human monocytes from healthy volunteers at 340C for 4 h was associated with inhibition of antigen presentation as assessed by expression of HLA-DR. A recent cohort study evaluated the effectiveness of hypothermia (< 360 C) in patients with advanced ovarian cancer during resection. Hypothermia was associated with a significant reduction in overall survival, at 34 months versus 45 months.

Hạ thân nhiệt làm tăng khả năng tái phát ung thư
4. Retrospective clinical evidence on the association between regional anesthesia and cancer recurrence
Several retrospective analyzes regarding the effects of regional anesthesia in cancer surgery on recurrence, metastasis, and survival of several tumor types, yield conflicting evidence. These are summarized, along with subsequent analysis of several previous randomized, controlled trials (FARCTs) designed to evaluate noncancerous outcomes in Table 2.
A database study A recent large-scale study showed that the use of epidural analgesia in combination with general anesthesia in colorectal cancer surgery was associated with improved 5-year survival (61 vs. for patients under general anesthesia), but there was no difference in cancer recurrence as assessed by chemotherapy or radiation therapy. Perhaps the effects of regional anesthesia are tumor-specific, however, differences remain. Retrospective studies are inherently susceptible to bias selection and are only useful for highlighting associations and generating hypotheses. Only prospective, multicenter, randomized, controlled trials can confirm a causal link, and these trials are ongoing in several tumor types, summarized in Table 3.
Table 3. Future: summary of several prospective, randomized, clinical trials being performed by the Outcome Research Consortium, Cleveland, OH
5. Conclusion
Some, but not all, experimental, animal, and retrospective evidence suggest an association between anaesthesia and cancer recurrence, but only prospective, randomized clinical trials, can demonstrate a cause-and-effect relationship. Patients with ongoing primary cancer, randomized to receive antineoplastic anesthesia (including regional anesthesia plus Propofol-based general anesthesia) or standard general anesthesia with opioid analgesia, and the results are eagerly awaited; this needs another 3-7 years. Meanwhile, there is no evidence to support a change in current routine clinical anesthesia practice in patients undergoing cancer surgery.
Composition according to A ́. Heaney1 and D. J. Buggy, “Can anaesthetic and analgesic techniques affect cancer recurrence or metastasis?”, British Journal of Anaesthesia 109 (S1): i17–i28 (2012) doi:10.1093/bja/aes421





