After venous thrombosis: How should it be treated?
The article is professionally consulted by Master, Doctor Do Nguyen Thuy Doan Trang - Head of Extracorporeal Circulation Team - Cardiovascular Center - Vinmec Central Park International General Hospital.
Post-VTE syndrome is very common after a deep vein thrombosis of the lower extremities. Therefore, it is necessary to prevent deep vein thrombosis of the lower extremities as well as to recognize the clinical signs to diagnose the post-thrombotic syndrome, contributing to the indications for treatment.
1. How dangerous is venous thrombosis?
Venous thromboembolism is very dangerous for patients because it can cause pulmonary embolism complications because blood clots form and develop in large veins in the legs or, in some cases, the arms. The thrombus then sloughs off and floats freely out of the deep veins, slowly traveling through the bloodstream and settling in the lungs, blocking blood circulation in the lungs, thereby causing the heart and lungs to work harder. Pulmonary embolism due to venous thrombosis is a medical emergency, large embolism can lead to death in a very short time for the patient.
Symptoms of venous thrombosis include:
Pain: A feeling of severe pain in the afternoon, often accompanied by symptoms of edema. Pain is often intermittent due to proximal obstruction, decompensation and a feeling of heaviness in the legs when walking, forcing you to stop to rest before symptoms subside. Edema: Symptoms of edema often appear early. Edema is usually white, tender and unilateral. Later, the edema becomes stiff and does not subside when the patient elevates the leg. Skin lesions: In addition to the symptoms of pain and edema, the patient also has lesions on the skin such as inflammation, fibrosis, atrophy, skin ulcers, etc. Superficial varicose veins: This symptom is usually on the obstructed side, in some cases Superficial varicose veins can be in the pelvis or abdomen. As a very dangerous syndrome, so the diagnosis to recover from venous thrombosis is very important in preventing dangerous complications of the disease.
Symptoms of venous thrombosis include:
Pain: A feeling of severe pain in the afternoon, often accompanied by symptoms of edema. Pain is often intermittent due to proximal obstruction, decompensation and a feeling of heaviness in the legs when walking, forcing you to stop to rest before symptoms subside. Edema: Symptoms of edema often appear early. Edema is usually white, tender and unilateral. Later, the edema becomes stiff and does not subside when the patient elevates the leg. Skin lesions: In addition to the symptoms of pain and edema, the patient also has lesions on the skin such as inflammation, fibrosis, atrophy, skin ulcers, etc. Superficial varicose veins: This symptom is usually on the obstructed side, in some cases Superficial varicose veins can be in the pelvis or abdomen. As a very dangerous syndrome, so the diagnosis to recover from venous thrombosis is very important in preventing dangerous complications of the disease.
2. Diagnosis of venous thrombosis
Diagnosis of venous thrombosis is usually based on clinical signs and symptoms as above. In addition, to make an accurate diagnosis, the doctor will appoint the following methods:
Doppler ultrasound: This is a subclinical exploration technique often prescribed by doctors first in the diagnosis of venous thrombosis. However, before performing ultrasound, both deep and superficial veins should be explored. If complete, or incomplete, thrombus is found on ultrasound, there may be signs of obstructive syndrome. In cases where the vein wall is thick, stiff, ECHO-dense, and irregular on ultrasound imaging, it may be a warning sign of a restrictive syndrome. In the case of patients with severe symptoms, unable to wear compression stockings, elastic bandages or patients who are expected to have surgery or intervention, it is necessary to appoint additional investigations such as: Contrast venography X-ray (including 2 methods: retrograde angiography and downstream angiography), intravascular ultrasound (is the optimal exploration method before conducting endovenous intervention in post-venous thrombosis syndrome). ) or an MRI scan.
Doppler ultrasound: This is a subclinical exploration technique often prescribed by doctors first in the diagnosis of venous thrombosis. However, before performing ultrasound, both deep and superficial veins should be explored. If complete, or incomplete, thrombus is found on ultrasound, there may be signs of obstructive syndrome. In cases where the vein wall is thick, stiff, ECHO-dense, and irregular on ultrasound imaging, it may be a warning sign of a restrictive syndrome. In the case of patients with severe symptoms, unable to wear compression stockings, elastic bandages or patients who are expected to have surgery or intervention, it is necessary to appoint additional investigations such as: Contrast venography X-ray (including 2 methods: retrograde angiography and downstream angiography), intravascular ultrasound (is the optimal exploration method before conducting endovenous intervention in post-venous thrombosis syndrome). ) or an MRI scan.
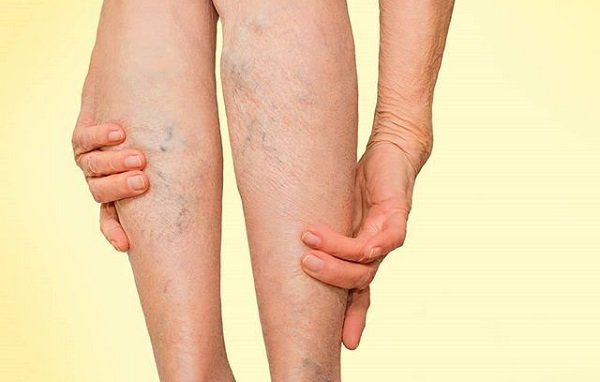
Để chẩn đoán huyết khối tĩnh mạch thường dựa vào các dấu hiệu triệu chứng lâm sàng
3. How to manage after venous thrombosis?
After venous thrombosis, it is necessary to prevent deep vein thrombosis of the lower extremities. Simultaneously, secondary prevention and prevention of progression to post-VTE syndrome are achieved by fibrinolytic therapy, acute venous thrombosis, and low-pressure compression stockings/elastics. at least 6 months. In addition, the management and recovery after venous thrombosis include the following supportive treatment methods:
Medical treatment:
Using elastic bandages, pressure socks: This is considered a first choice in the treatment and recovery of venous thromboembolism. Normally the pressure used is 20-30 mmHg. However, this method affects the quality of life of patients. Using intravenous drugs: When using intravenous drugs, the patient will feel more comfortable because the symptoms are relieved. Other measures such as: Inflating pressure from time to time, postural drainage, lymphatic drainage... or using antibiotics when there is inflammation and superinfection... Surgical intervention:
Surgical failure Superficial veins: For saphenous veins, surgery, or intervention to treat saphenous vein reflux by compensating the saphenous vein system is usually small, but the effect is only temporary. For perforated veins, it can be treated with endoscopic surgery, perforated vein ligation or sclerotherapy, endovenous intervention. Surgical treatment of deep vein insufficiency : Including methods such as repair of the venous valve, transposition of a vein with insufficiency of a healthy venous valve or grafting a segment of a vein with a valve into a diseased vein, creating a new venous valve Treatment Deep vein insufficiency: In the case of deep venous reflux, it is necessary to determine whether the cause is a consequence of venous thrombosis or not. Usually, phlebotomy is indicated in non-thrombotic deep venous insufficiency after other treatments have failed. Treatment of chronic deep vein occlusion: The location of veins that need intervention is the inferior vena cava, the iliac vein, and the femoral vein. The treatment methods are femoral-femoral (Palma) bypass surgery, thigh-pelvis, femoral-host or possibly dilatation and venous stenting Treatment of deep vein thrombosis: Endovenous interventions such as: dilation, stent placement. These are the methods of first choice in the treatment of iliac-femoral venous stenosis due to deep vein thrombosis. Normally, intravenous dilation and stenting are usually indicated for patients with severe symptoms such as edema, skin changes, etc., when appropriate bandages/compression stockings are used but the symptoms do not improve. In summary, post-VTE syndrome is very common after DVT of the lower extremities. Therefore, it is necessary to prevent deep vein thrombosis of the lower extremities as well as to recognize the clinical signs to diagnose the post-thrombotic syndrome, contributing to the indications for treatment.
Medical treatment:
Using elastic bandages, pressure socks: This is considered a first choice in the treatment and recovery of venous thromboembolism. Normally the pressure used is 20-30 mmHg. However, this method affects the quality of life of patients. Using intravenous drugs: When using intravenous drugs, the patient will feel more comfortable because the symptoms are relieved. Other measures such as: Inflating pressure from time to time, postural drainage, lymphatic drainage... or using antibiotics when there is inflammation and superinfection... Surgical intervention:
Surgical failure Superficial veins: For saphenous veins, surgery, or intervention to treat saphenous vein reflux by compensating the saphenous vein system is usually small, but the effect is only temporary. For perforated veins, it can be treated with endoscopic surgery, perforated vein ligation or sclerotherapy, endovenous intervention. Surgical treatment of deep vein insufficiency : Including methods such as repair of the venous valve, transposition of a vein with insufficiency of a healthy venous valve or grafting a segment of a vein with a valve into a diseased vein, creating a new venous valve Treatment Deep vein insufficiency: In the case of deep venous reflux, it is necessary to determine whether the cause is a consequence of venous thrombosis or not. Usually, phlebotomy is indicated in non-thrombotic deep venous insufficiency after other treatments have failed. Treatment of chronic deep vein occlusion: The location of veins that need intervention is the inferior vena cava, the iliac vein, and the femoral vein. The treatment methods are femoral-femoral (Palma) bypass surgery, thigh-pelvis, femoral-host or possibly dilatation and venous stenting Treatment of deep vein thrombosis: Endovenous interventions such as: dilation, stent placement. These are the methods of first choice in the treatment of iliac-femoral venous stenosis due to deep vein thrombosis. Normally, intravenous dilation and stenting are usually indicated for patients with severe symptoms such as edema, skin changes, etc., when appropriate bandages/compression stockings are used but the symptoms do not improve. In summary, post-VTE syndrome is very common after DVT of the lower extremities. Therefore, it is necessary to prevent deep vein thrombosis of the lower extremities as well as to recognize the clinical signs to diagnose the post-thrombotic syndrome, contributing to the indications for treatment.

Sau khi bị huyết khối tĩnh mạch cần phải dự phòng huyết khối tĩnh mạch sâu chi dưới
At Vinmec International General Hospital, diagnostic imaging plays a very important role when implementing examination and treatment of venous thrombosis. Under the guidance of ultrasound machine, MRI machine, CT computerized tomography machine, modern DSA angiography room, the injury site will be identified and approached in many different directions. From here, doctors can quickly come up with a treatment plan for the patient. Not only has a modern equipment system, Vinmec is also a place to gather a team of experienced doctors and nurses who will greatly assist in the diagnosis and early detection of abnormal signs of the body. In particular, with a space designed according to 5-star hotel standards, Vinmec ensures to bring patients the most comfort, friendliness and peace of mind.
Để đặt lịch khám tại viện, Quý khách vui lòng bấm số HOTLINE hoặc đặt lịch trực tiếp TẠI ĐÂY. Tải và đặt lịch khám tự động trên ứng dụng MyVinmec để quản lý, theo dõi lịch và đặt hẹn mọi lúc mọi nơi ngay trên ứng dụng.
Bài viết này được viết cho người đọc tại Sài Gòn, Hà Nội, Hồ Chí Minh, Phú Quốc, Nha Trang, Hạ Long, Hải Phòng, Đà Nẵng.






