This article has been professionally reviewed by Dr. Nguyen Van Dinh – Head of the Respiratory – Asthma – Allergy – Clinical Immunology Unit, Vinmec Times City International Hospital.
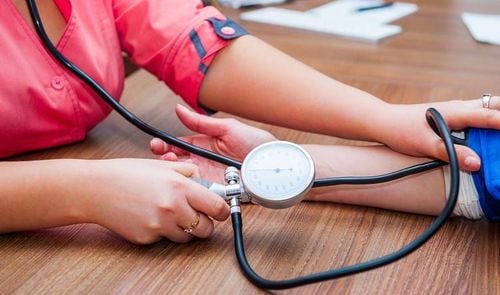
Hypertension is a common condition in adults with bronchial asthma. There are several methods to improve blood pressure in asthma patients. However, some medications carry the risk of triggering asthma attacks or exacerbating the disease. Therefore, which treatment should be prioritized for lowering blood pressure in patients with both bronchial asthma and hypertension?
Hypertension Symptoms Are Often Subtle (e.g., headache, nosebleeds), and in many cases, patients with bronchial asthma are diagnosed with hypertension during routine check-ups.
Hypertension is often referred to as a "silent killer" because it quietly leads to cardiovascular complications. When combined with bronchial asthma, poorly controlled hypertension can result in severe complications, such as:
- Stroke
- Coronary artery disease
- Heart failure
- Increased mortality rate
- Prolonged hospitalization in asthma patients
1. Relationship Between Bronchial Asthma and Hypertension
The mechanism of bronchial asthma involves inflammatory factors, leading to airway inflammation and swelling, which narrows the airways. This, combined with hyperresponsiveness of bronchial smooth muscles, results in difficulty breathing for asthma patients.
There is no clear mechanism linking bronchial asthma to hypertension and cardiovascular diseases. However, some studies suggest that inflammatory mediators may play a role.
- During an asthma attack, difficulty breathing leads to hypoxia, increased heart rate, and sympathetic overactivity, causing temporary hypertension.
- Improper treatment or prolonged use of corticosteroids in high doses can lead to hypertension and systemic side effects.
Conversely, some antihypertensive medications, such as non-selective beta-blockers, ACE inhibitors, and aspirin, can worsen asthma control and trigger acute bronchospasms.
Thus, the management of both bronchial asthma and hypertension should be carefully guided by a specialist. Patients should not discontinue or modify medications without medical advice.
2. Non-Pharmacological Methods for Hypertension Management
Lifestyle changes play a crucial role in controlling both hypertension and bronchial asthma:
- Regular, gentle exercise and maintaining an ideal body weight. Weight loss should follow a doctor’s guidance.
- Aim for at least 30 minutes of exercise, 4 times a week.
- Adopting a healthy diet:
- Reduce intake of fried, greasy, and salty foods.
- Increase vitamin and fiber intake from fruits and vegetables (while avoiding allergens).
- Quit smoking and avoid stimulants. Encourage family members to create a smoke-free environment.
- Limit exposure to dust, cold air, and environmental pollutants.
- Do not self-medicate without a doctor’s prescription.
- Monitor blood pressure at home following the doctor’s instructions. Frequent monitoring is not necessary to avoid excessive anxiety.

3. Selecting Antihypertensive Medications for Asthma Patients
Medications to Use with Caution in Asthma Patients
Beta-Blockers
- Non-selective beta-blockers (e.g., Propranolol, Carvedilol) are contraindicated in asthma patients. These drugs act on both cardiac and bronchial beta receptors, causing bronchoconstriction, reducing the effectiveness of bronchodilators, and triggering or worsening acute asthma attacks.
- Selective beta-blockers mainly target the cardiovascular system, but some studies show they may slightly reduce lung function.
- However, for patients with a history of coronary artery disease or systolic heart failure, selective beta-blockers may still be considered if asthma is mild to moderate.
ACE Inhibitors
- ACE inhibitors may cause persistent dry cough, occurring in up to 20% of patients.
- There is debate over whether this cough can trigger acute asthma exacerbations.
- While not strictly contraindicated, ACE inhibitors are not the first choice for asthma patients.
Safe Antihypertensive Medications for Asthma Patients
Diuretics:
- Some diuretics may cause hypokalemia (low potassium levels), while bronchodilators have a similar side effect.
- Potassium levels should be monitored when using diuretics in asthma patients.
Calcium Channel Blockers (e.g., Nifedipine, Nicardipine):
- Besides lowering blood pressure, these drugs have a theoretical advantage in asthma:
- Relax bronchial smooth muscles.
- Inhibit mast cell degranulation, reducing allergic responses.
- Enhance the bronchodilatory effects of beta-agonists.
- Low-dose thiazide diuretics alone or in combination with calcium channel blockers are preferred antihypertensive strategies for asthma patients.
Angiotensin II Receptor Blockers (ARBs)
4. Preventing Hypertension in Asthma Patients
The best preventive approach is to modify controllable risk factors:
- Adopt a healthy lifestyle.
- Manage associated conditions such as dyslipidemia and diabetes.
Ensure optimal asthma control to:
- Reduce cardiovascular risks.
- Minimize asthma exacerbations.
- Prevent medication side effects that may increase cardiovascular risk.
Increase awareness about disease prevention and strictly follow medical treatment plans for both hypertension and asthma.
🔗 [Read more: Guidelines for Diagnosis and Treatment of Bronchial Asthma]
For more health, nutrition, and beauty tips, visit Vinmec International General Hospital to safeguard the health of yourself and your loved ones.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.