This article was written by Dr. Lê Thị Thu Hằng, Specialist level I in Dermatology at the Department of Outpatient & Internal Medicine, Vinmec Hai Phong International General Hospital.
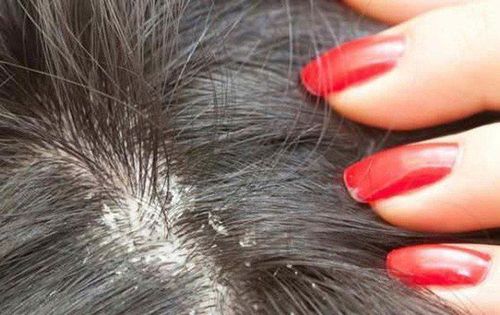
Tinea capitis is an inflammatory condition that causes damage to the hair, hair follicles, scalp, and surrounding skin due to fungi. It is mainly found in children but is rarer in adults. The disease is more common in rural areas than in urban settings, and it is contagious.
1. Causes of Tinea Capitis
• Dermatophyte fungi are the primary cause of tinea capitis. The most common fungi involved are Microsporum and Trichophyton. In the UK and North America, Trichophyton tonsurans is the most common cause, accounting for 90% of cases. However, studies in Vietnam show that M. canis is more commonly found.
• Piedra white hair fungus is caused by Trichophyton beigelii, while Piedra black hair fungus is caused by Piedraia hortae. Along with the HIV pandemic, the incidence of Piedra hair fungus has increased. In addition to affecting the hair, Piedra can also cause systemic fungal infections and damage internal organs.
Classification of dermatophyte is based on how it spreads
2. Symptoms of Tinea Capitis
2.1 Clinical Features
• Piedra Fungus: There are two main forms—Black Piedra and White Piedra.
- In Black Piedra, the patient typically presents with brown or black nodules along the hair shaft. The infection usually starts beneath the cuticle of the hair and spreads outward. Hair breakage may occur as the nodules rupture along the hair shaft.
- In White Piedra, the infection also starts beneath the cuticle and spreads along the hair shaft, causing weakness and breakage. The nodules are soft, non-adherent, and may appear white, red, green, or light brown. The incidence of White Piedra has increased since the onset of the HIV epidemic. In immunocompromised individuals, T. beigelii can cause severe systemic fungal infections, including fever, candidemia, lung infiltration, skin lesions (such as vesicular and hemorrhagic rashes, central necrosis), and kidney disease.
• Tinea Capitis (Scalp Ringworm):
Symptoms can range from mild, non-inflammatory forms resembling seborrheic dermatitis (commonly caused by T. tonsurans) to severe pustular reactions with hair loss, a condition known as kerion (honeycomb-like). Hair loss may or may not be accompanied by flaking skin.
• Kerion results from an exaggerated immune response, leading to pustular lesions, small abscesses, and hair loss. Some patients may have systemic symptoms, such as fatigue and swollen lymph nodes. Hair in the affected area may regrow; however, if the lesions persist, they can leave scars and cause permanent hair loss.
• Carrying the T. tonsurans fungus without symptoms (asymptomatic carrier) is common in adults, especially those who have been in contact with infected children. These carriers should be treated to prevent the disease from spreading to children.

Dermatophytes infiltrate and reside in the hair in three forms: intracellular, extracellular, and favus.
• Extracellular form: The outer layer of the hair shaft is destroyed. Infected hairs may fluoresce under Wood's light (due to Microsporum) or may not (due to Microsporum and Trichophyton). The clinical presentation varies from flaky patches to bald spots with inflammation, ranging from mild to severe, sometimes forming kerion.
• Favus: This is the most severe form of dermatophyte infection in the hair. It is primarily caused by T. Schoenleinii. Under Wood's light, it shows a pale blue fluorescence. The lesions appear as yellow crusted patches, thickened with hyphae and dead skin. Chronic infections can cause permanent hair loss and scarring.
2.2 Paraclinical Testing
• Direct Microscopy: Examine scalp and hair samples (scales and hair). Use KOH (10-20%) with blue ink for direct microscopy. Fluorescent dyeing with acridine orange, calcofluor white, and blankophor can be used under fluorescence microscopy to detect fungal polysaccharides. On direct slides, fungal hyphae with septations and branching will be visible.
• Culture: The basic culture medium is Sabouraud agar. Cultures take 7-14 days to confirm a positive result and up to 21 days for a negative result.

2.3 Treatment
• Principles:
- Cut hair short.
- Wash the scalp with antifungal and antiseptic solutions.
- Use antifungal medications carefully and monitor closely.
- Treat any coexisting bacterial infections.
• Specific Treatment:
- Piedra Fungus: Remove infected hair and wash the scalp with sulfur-based shampoo. Ketoconazole 2% or oral terbinafine can be effective.
Tinea Capitis:
Adults: Use one of the following medications:
Fluconazole 6mg/kg/day for 3-6 weeks.
Griseofulvin 20mg/kg/day for 6-8 weeks.
Itraconazole 5mg/kg/day for 4-8 weeks.
Terbinafine 250mg/day for 2-4 weeks.

Children: Use one of the following medications:
Fluconazole 6mg/kg/day for 6 weeks.
Griseofulvin 20-25mg/kg/day for 6-8 weeks.
Itraconazole 3-5mg/kg/day for 6 weeks.
Terbinafine 62.5mg/day (<20kg), 125mg/day (20-40kg), or 250mg/day (>40kg) for 2-6 weeks.
3. Prevention of Tinea Capitis
• Regular hair hygiene.
• Avoid washing hair at night.
• Keep hair dry.
• Limit young children’s interaction with animals.

Vinmec International General Hospital is a healthcare facility that ensures high-quality services, offering expert medical advice and care, with state-of-the-art equipment and a safe, hygienic environment. Patients can be confident in the accuracy of their test results. For any health concerns, patients should seek consultation from specialized doctors.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.