Article consulted by Master's Degree, Doctor Nguyễn Thị Nhật - Infectious Disease Specialist - Internal Medicine & Outpatient Department - Vinmec Hai Phong International Hospital.
Intravenous injection is a technique that uses a syringe to deliver medication into the body via a vein to rapidly achieve the desired effect.
1. Indications/Contraindications for Intravenous Injection
Intravenous injection is a technique that uses a syringe to deliver medication into the body via a vein to rapidly achieve the desired effect.
1.1. Indications for Intravenous Injection:
- Emergency patients;
- Malnourished patients;
- Patients in critical condition requiring rapid drug effects: anesthetics, sedatives, hemorrhage control, treatment of shock, etc.;
- Medications that may cause tissue necrosis, are not absorbed, or are destroyed by the digestive tract;
- Medications for systemic effects;
- When a large volume of medication is required;
- Medications that cannot be administered intramuscularly or subcutaneously, which can only be given intravenously;
- Blood, plasma, and colloidal solutions like Dextran;
- Therapeutic serums;
- Patients who cannot take oral medication: those with persistent vomiting, pre-surgical preparation, or uncooperative attitude.

1.2. Contraindications for Intravenous Injection:
- Oil-soluble medications or rapid intravenous injection drugs that could cause arrhythmias;
- Medications that strongly stimulate the cardiovascular system, such as adrenaline (should only be administered intravenously in emergencies when blood pressure is critically low or not detectable);
- Absolute contraindications for intravenous injection at sites that are infected or burned;
- Relative contraindications for intravenous injection in paralyzed limbs, areas of edema, and joints.
1.3. Injection Sites:
- Head veins: both temples;
- Limb veins: back of the hands, wrists, elbows, back of the feet, ankles, etc.;
- It's advisable to choose larger, more visible, and less mobile veins.
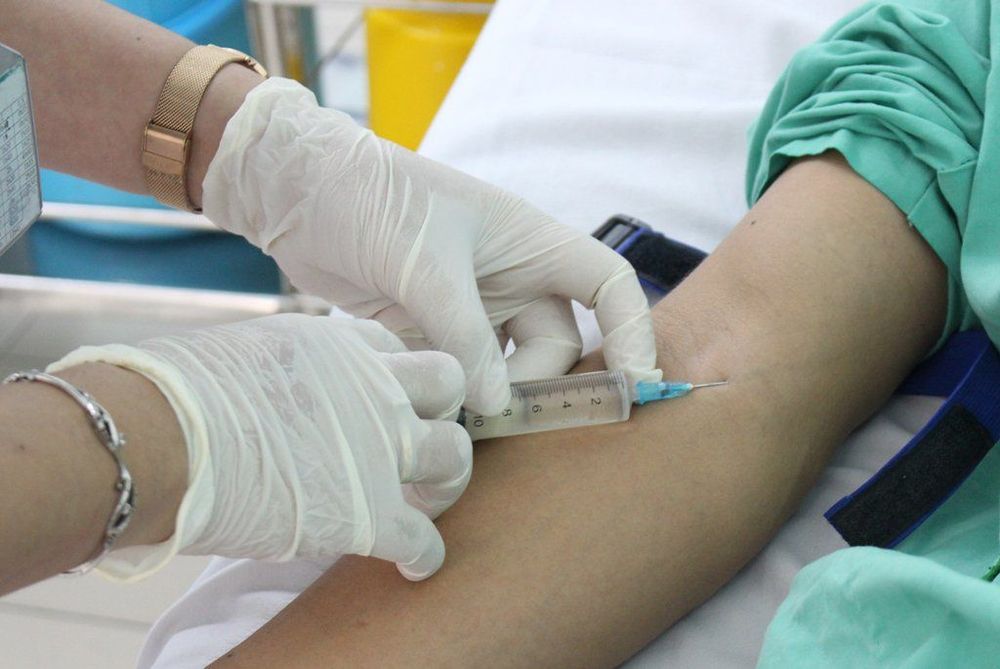
2. Intravenous Injection Technique
2.1. Preparation:
- Nurse: Wash hands and wear appropriate attire;
- Patient and family: Explain the intravenous injection process, inquire about allergy history, perform antibiotic testing as indicated, assess vital signs;
- Prepare equipment: including sterile tools (sterile tray, appropriate syringe, forceps, forceps holder, cotton, disposable container), clean tools (gloves, 70° alcohol, tourniquet, shock kit) and medical records, waste container, etc.;
- Prepare medications: injectable drugs, solvents, distilled water, 5% glucose if indicated for drug preparation.
2.2. Intravenous Injection Process:
Carry out the injection according to the "5 rights" principle: right patient, right drug, right route, right dose, right time. The intravenous injection procedure includes:
- Wash hands, disinfect them, disinfect the vial cap and solvent;
- Prepare the medication, shake well, observe its color and characteristics to ensure optimum quality for use;
- Withdraw the medication according to the prescription;
- Identify the appropriate injection site, tighten the tourniquet if necessary, and disinfect the injection site with cotton soaked in 70% alcohol, allowing the skin to dry;
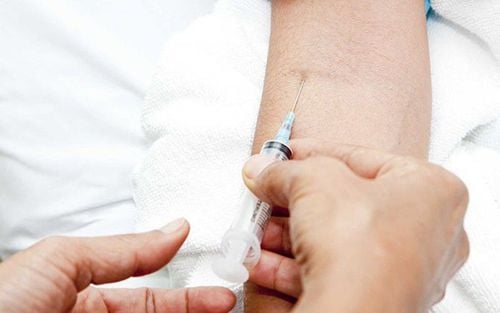
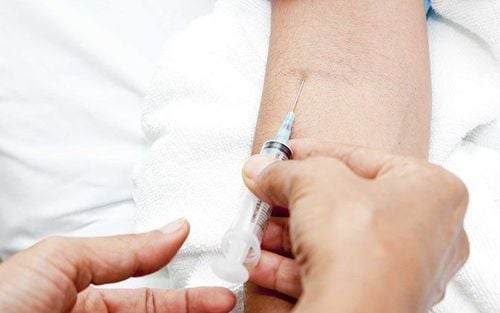
- Insert the needle into the vein;
- Remove the tourniquet and slowly inject the medication while closely monitoring the patient;
- Quickly withdraw the needle, apply pressure with cotton at the injection site after administering the medication;
- Assist the patient in a comfortable position, instruct the patient and family to watch for any abnormal signs in complexion, consciousness, respiratory condition, etc.;
- Clean up the equipment, wash hands, and record in the medical records.
2.3. Monitoring During and After Intravenous Injection:
- Monitor during the injection: Observe the patient's facial appearance; if there are signs of anaphylactic shock, stop the injection immediately and notify the doctor for appropriate action. Additionally, issues like blocked needles, swelling at the injection site, or patient anxiety may arise, necessitating prompt intervention;
- Post-injection monitoring: Monitor closely for delayed allergic reactions like rashes at the injection site or other parts of the body.

2.4. Complications and Management of Intravenous Injection:
- Blocked Needle: Caused by blood clotting in the needle tip, preventing the administration of medication. The management involves withdrawing the needle from the injection site, pushing the syringe plunger to release blood, and if necessary, switching to a new needle;
- Swelling at the Injection Site: Occurs when the needle punctures the vein or part of the bevel is partially in the vessel and partially outside. To manage, withdraw the needle and re-inject; afterward, apply a warm compress to help disperse any accumulated blood and expedite drug absorption;
- Vascular Occlusion: Results from air entering the bloodstream through the syringe or injecting an inappropriate oil-based medication. To prevent this, ensure no air remains in the syringe before administering and avoid using the wrong medications;
- Patient Fainting or Panic: Effective psychological preparation for patients before the intravenous injection is crucial. If a patient faints due to fear, adverse medication reactions, or repeated unsuccessful attempts to find a vein, stop the injection and seek medical assistance;
- Infection: Due to poor aseptic technique or prolonged catheterization. Preventive measures to reduce the risk of infection include maintaining good aseptic practices before, during, and after administering medication to patients, and being mindful of the duration of catheterization.
- Necrosis: Caused by injecting substances contraindicated for subcutaneous or intramuscular injection outside the vein. Symptoms include warmth, redness, pain at the injection site, initially firm, then soft. The appropriate management is warm compresses; if there is significant necrosis, it should be bandaged lightly to prevent further infection, and large areas of necrosis may require incision and drainage.
• Anaphylactic shock: Caused by the body’s reaction to the administered medication. Symptoms of anaphylactic shock include restlessness, fear, lethargy or coma, rapid and weak pulse, difficulty breathing, cyanosis, itching, rash, and hives. The immediate response is to stop the injection and manage according to the anaphylactic shock emergency protocol.
• Viral infections (HBV, HCV, HIV): HBV and HCV infections can be transmitted through poorly sterilized syringes and needles from hepatitis patients to healthy individuals (with detection occurring 4 - 6 months after injection, manifesting as fatigue, jaundice, loss of appetite, and dark urine); HIV transmission can occur from unsanitary intravenous injections. Treatment is determined by the physician based on specific cases.
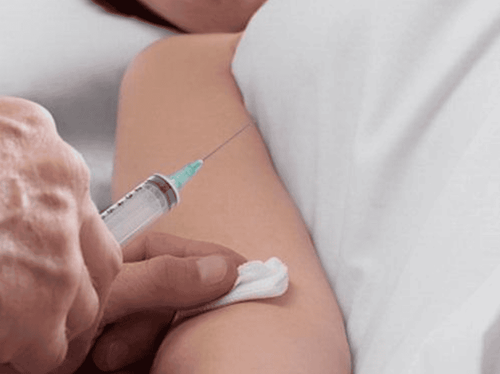
3. Intravenous infusion technique with catheter lock
The intravenous catheter technique involves injecting or infusing into the vein using a soft plastic cannula inserted into the bloodstream and securely fixed inside, with a non-sharp tip that prevents piercing the vessel wall.
This technique is used when patients require multiple injections or infusions throughout the day or need prolonged intravenous treatment. Peripheral intravenous catheters overcome the drawbacks of metal needles, such as vein misplacement, vessel perforation, and pain during administration.
3.1 Indications/Contraindications:
Indications:
- Patients requiring emergency resuscitation: shock, circulatory collapse, coma, respiratory failure, cardiac arrest, etc.;
- Continuous fluid infusion;
- Intermittent fluid infusion;
- Intravenous drug injections and infusions;
- Blood transfusions and blood products;
- Before procedures, surgeries, or the use of contrast agents, etc.;
- Cases needing short-term intravenous nutrition.
Contraindications:
- Damaged, infected, bruised, or burned vein areas.
3.2 Performing the technique
- Inform and explain the procedure to the patient and their family;
- Inquire about drug allergies;
- The nurse should wear a mask and perform hand hygiene;
- Prepare equipment similar to intravenous injections;
- Check the "5 rights" principle;
- Position the patient appropriately, exposing the injection site;
- Sterilize hands, wear clean gloves, and disinfect the catheter lock;
- Check the cannula, administer the medication;
- Flush the catheter lock with saline;
- Withdraw the needle, apply cotton to the catheter lock, and cover the needle tip with a sterile dressing;
- Instruct the patient and their family on how to monitor after IV infusion;
- Clean up the equipment and document in the medical record.
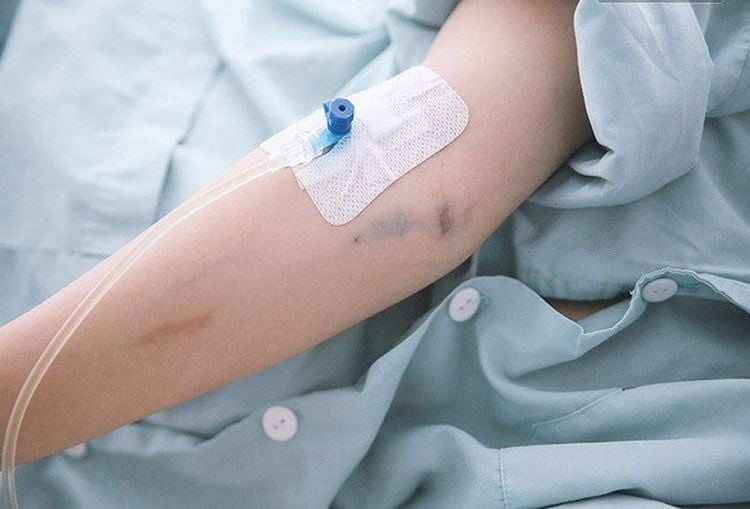
3.3 Monitoring:
- Monitor the patient's appearance and condition during and after the procedure;
- Care for the catheter every 8 - 12 hours or according to the patient's actual condition;
- Check the insertion site daily;
- Do not keep the catheter for more than 3 days;
- If any signs such as catheter blockage, swelling, warmth, redness, pain along the vein, bleeding at the site, or infection occur, withdraw the catheter and change the insertion site.
3.4 Complications and management:
- Accidental artery puncture: immediately withdraw the needle, apply pressure at the puncture site, and monitor for local bleeding to follow appropriate steps.
- Extravasation: caused by catheter misplacement or vein rupture, withdraw the infusion needle, move to another site, and monitor frequently while notifying the physician for proper management.
- Hematoma: due to bleeding around the tissue or the needle penetrating the blood vessel. Management includes withdrawing the infusion needle and applying a cold compress around the hematoma.
- Catheter dislodgement: may occur due to improper fixation or self-removal by the patient, handled by withdrawing the infusion needle.
- Phlebitis: caused by the formation of a blood clot at the catheter tip, prolonged catheter use, or infusions with an inappropriate pH. Management involves withdrawing the infusion needle, warm compresses, and notifying the physician for necessary adjustments.
- Local infection: managed by withdrawing the infusion needle, changing the IV site to another limb, informing the treating physician, and monitoring and caring for the infected site according to the treatment protocol.
- Systemic infection: can result from poor aseptic techniques, insufficient care of the IV site, prolonged catheter use, prolonged phlebitis, or immune-compromised conditions. In this case, notify the physician for the necessary medication and monitor vital signs and the patient's overall condition.
- Other complications include venous spasm, circulatory overload, drug allergies, ligament damage, nerve injury, or air embolism. Appropriate management should follow the prescribed treatment protocol.
4. Important notes for intravenous infusion using a catheter lock
- Use sterile gauze to cover the catheter insertion site.
- Change the dressing and gauze every 24 to 48 hours or immediately if the dressing is damp or compromised.
- It is necessary to rotate the catheter insertion site every 48 to 72 hours. If it is not possible to change the site, inform the doctor to take appropriate measures.
- If the catheter is not needed, it should be removed immediately.
When instructed to perform intravenous injection, the patient should cooperate with healthcare staff to ensure effective treatment.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.