This article was professionally consulted by a Hematology - Blood Transfusion specialist from the Laboratory Department of Vinmec Ha Long International General Hospital.
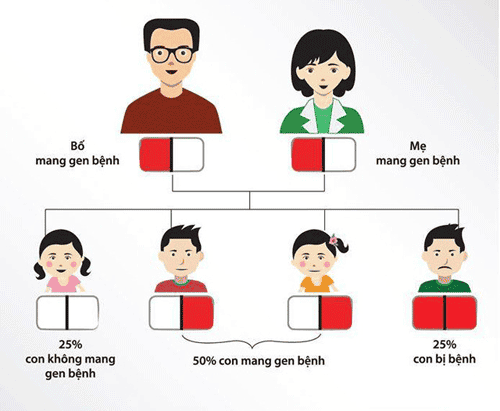
Thalassemia is a hereditary hemolytic disorder inherited in an autosomal recessive pattern, passed from parents to children through generations. The primary manifestation of the disease is anemia, which can lead to severe complications and significantly impact the genetic health of a population. Undergoing pre-marital screening tests is essential for accurately detecting Thalassemia genes, determining whether prospective parents are carriers, and assessing the potential risk of Thalassemia in their future children.
1. What is Thalassemia?
Thalassemia, or congenital hemolytic anemia, is caused by an abnormal structure of hemoglobin in red blood cells. This leads to reduced red blood cell quality, making them more fragile and prone to rupture (hemolysis), resulting in chronic anemia. In severe cases, patients often require regular blood transfusions. However, frequent transfusions can lead to iron overload, causing complications in multiple organs and altering the patient’s physical appearance resulting in short stature, prominent forehead, flat nose, protruding teeth, as well as heart failure, liver failure, endocrine disorders, and even death.
There are different types of Thalassemia, classified based on the type and number of mutated genes. In Vietnam, the two most common forms are Alpha Thalassemia (caused by a loss-of-function mutation in the Alpha-globin gene) and Beta Thalassemia (caused by a loss-of-function mutation in the Beta-globin gene).
2. Why is pre-marital screening for Thalassemia necessary?
Currently, approximately 7% of the global population carries the Thalassemia gene, and 1.1% of couples are at risk of having children with the disease or being carriers.
According to the National Institute of Hematology and Blood Transfusion (Vietnam), Vietnam is among the countries with a high prevalence of Thalassemia gene carriers, with 10% of the population carrying the gene. It is estimated that around 8,000 children with Thalassemia are born each year in Vietnam, of whom 2,000 suffer from severe forms of the disease.
Children born with Thalassemia face serious health risks, including iron overload, enlarged spleen, infections, bone deformities, growth retardation, and cardiovascular diseases such as congestive heart failure and arrhythmias.
Currently, the primary treatment for Thalassemia involves lifelong blood transfusions and iron chelation therapy to manage iron overload. The cost of treatment is extremely high, and parents often have to take time off work to care for their hospitalized children, placing a significant financial and emotional burden on the family.
3. The severe consequences of Thalassemia
Most Thalassemia patients experience facial bone deformities due to excessive bone marrow expansion, particularly in the upper jaw. Their skin may develop a grayish discoloration, especially around the nail beds, elbows, knees, and ankles. The disease can also affect various organs in the body, including:
- Enlarged spleen (splenomegaly)
- Reduced platelet count (thrombocytopenia)
- Severe anemia
- Pathological fractures and early fusion of the lower epiphysis of the femur
- Pituitary gland: Impaired development of reproductive organs, adrenal glands, and thyroid gland
- Parathyroid gland: Low blood calcium levels (hypocalcemia)
- Liver: Hepatomegaly (enlarged liver)
- Pancreas: Increased risk of diabetes
- Reproductive system: Delayed or impaired sexual development and function
People with Thalassemia require lifelong blood transfusions, relying on donated blood to survive. Despite its severity, Thalassemia is a preventable disease through prenatal and pre-marital screening.
4. Pre-marital health screening – the only preventive solution
Given the serious consequences of Thalassemia, it is essential to have accurate diagnostic standards, effective treatment methods, and reliable screening strategies. Doctors diagnose the disease based on clinical symptoms, complete blood count (CBC), and biochemical tests, allowing them to determine the most appropriate treatment approach.
To prevent passing Thalassemia to future generations, couples are strongly advised to take the following steps before marriage:
- Pre-marital counseling: Couples planning to marry should undergo screening and testing for Thalassemia before getting married.
- Family screening: Relatives of Thalassemia patients should also be screened.
- Genetic counseling for carrier couples: If both partners carry the same type of Thalassemia gene, they should seek genetic counseling before planning for pregnancy.
- If a Thalassemia carrier couple conceives, fetal screening should be performed between 12 and 18 weeks of pregnancy at a specialized medical facility.
- Consult specialists: Couples should seek advice from Hematology, Pediatrics, and Genetics specialists to fully understand the risks and management of Thalassemia.
5. Pre-marital screening tests for assessing the risk of Thalassemia in children
Pre-marital screening tests help identify Thalassemia carriers, allowing for an assessment of the risk of passing the disease to future generations. These tests include:
5.1. Screening tests
These tests do not provide a definitive diagnosis of carrier status but help identify individuals at high risk of carrying Thalassemia genes. Common screening tests include:
- Complete blood count (CBC) test using automatic or semi-automatic hematology analyzers to measure: Red blood cell (RBC) count, Hemoglobin (Hb) levels, Mean corpuscular hemoglobin (MCH), Mean corpuscular volume (MCV)
A carrier indication is suggested if MCH < 27 pg or MCV < 80 fL.
- Microscopic evaluation of red blood cell morphology and size: Identifying microcytic (small-sized) and hypochromic (pale) red blood cells under a microscope.
5.2. Confirmatory diagnostic tests
5.2.1. Hemoglobin identification and quantification
The most commonly used test samples include venous blood or dried blood spots, which can be collected from the heel, earlobe, or fingertip. In normal cases, hemoglobin percentages are as follows:
- Adults: HbA: 95-98%, HbA2: 2-3%, HbF: 0.8-2%, HbC: 0%
- Children:
- Newborns: HbF: 50-80%
- Infants (6 months old): HbF: 8%
- Children over 6 months: HbF: 1-2%
To identify hemoglobin types and percentages, the following laboratory techniques are commonly used:
- Gel electrophoresis or cellulose acetate electrophoresis
- Capillary electrophoresis - a more advanced technique performed using specialized automated electrophoresis machines with high resolution
- High-performance liquid chromatography (HPLC) - a modern, fast, and highly accurate method
5.2.2. Genetic testing
DNA analysis detects genetic mutations in the alpha and beta globin genes. This is done using sequencing techniques or polymerase chain reaction (PCR) with specific primers. This allows for the accurate identification of Thalassemia carriers.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.