Anal bleeding may be a warning sign of a gastrointestinal condition or specific anorectal diseases such as hemorrhoids, anal fissures, or malignant anorectal disorders. It typically presents as bright red or dark red blood passing from the anus. The severity of anal bleeding can range from mild to severe, depending on the underlying cause. This condition is commonly seen in outpatient settings; however, according to some reports, less than half of patients experiencing anal bleeding seek timely medical consultation and treatment.
1. What Is Anal Bleeding?
Anal bleeding refers to the passage of bright red blood from the anus, often mixed with stool and sometimes accompanied by blood clots. Blood in the stool may originate from the rectum, anus, or other parts of the gastrointestinal tract.
The severity of anal bleeding varies widely. Most cases are mild and stop on their own. Many patients report noticing only a few drops of bright red blood, which may turn the toilet water pink or appear as stains on toilet paper after wiping, often without any pain. In general, mild anal bleeding can be evaluated and treated in outpatient settings without the need for hospitalization or emergency intervention.
However, bleeding can also be moderate or severe. Patients with moderate bleeding may pass a larger amount of bright red or dark red blood, often mixed with stool and/or blood clots, during multiple bowel movements. Those with severe bleeding may experience multiple bowel movements containing a large volume of blood or a single bowel movement with significant blood loss. Moderate or severe rectal bleeding may cause symptoms such as weakness, dizziness, fainting, low blood pressure, or orthostatic hypotension. In such cases, hospitalization, emergency treatment, and possible blood transfusion may be required.
2. Common Causes of Anal Bleeding
Anorectal conditions are the most common causes of anal bleeding.
2.1 Hemorrhoids
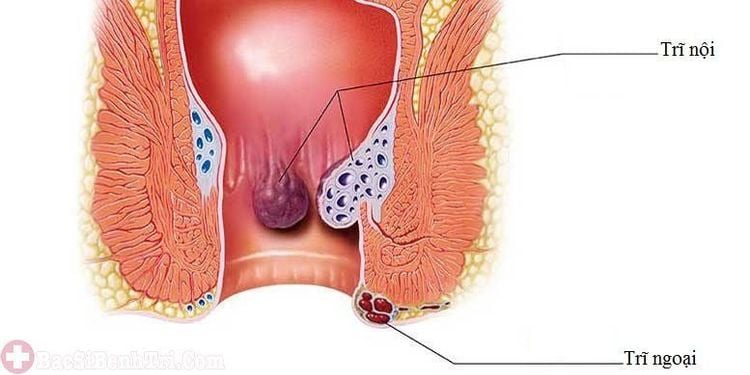
Hemorrhoids occur when the veins in the rectal and anal regions become swollen. The main symptoms of hemorrhoids include anal bleeding due to dilated hemorrhoidal veins, pain, discomfort, and itching.
Both internal and external hemorrhoids in the early stages may cause painless anal bleeding. Patients often first notice the condition when they feel a lump in the anal area during bowel movements.
Treatment for hemorrhoids focuses on symptom relief, such as using stool softeners. In cases where thrombosed hemorrhoids occur, blood clots form within the swollen veins, causing moderate to severe pain and requiring minor surgical removal of the hemorrhoidal tissue.
2.2 Anal Fissure
An anal fissure is a tear in the lining of the anal canal, usually caused by passing hard stool.
Anal fissures can lead to mild anal bleeding, with bright red blood. The tear in the mucosa exposes nerves and blood vessels, resulting in moderate to severe pain. The pain intensifies during bowel movements and gradually decreases between them.
For hemorrhoids and anal fissures, symptoms often improve with stool softeners, increased fiber intake, pain relievers, and regular warm baths.
2.3 Infections
Bacterial dysentery can cause diarrhea with blood in the stool. The pathogens responsible include Campylobacter jejuni, Salmonella, Shigella, Escherichia coli, and Clostridium difficile.
Symptoms include abdominal pain, fever, and bloody diarrhea. The condition is usually treated with antibiotics.
2.4 Inflammatory Bowel Disease (IBD)
Inflammatory bowel disease is a common cause of anal bleeding in adults, especially those under 50 years old. The two major types are Crohn's disease and ulcerative colitis.
Bleeding typically presents as small to moderate amounts of bright red blood in the rectum, often mixed with stool and mucus. Hospitalization is not always necessary, but rest and steroid treatment are commonly prescribed.
2.5 Angiodysplasia
This vascular condition involves enlarged veins and capillaries in the walls of the digestive tract, often occurring in the right colon. These blood vessels become fragile and can bleed.
Anal bleeding from angiodysplasia is often slow, chronic, and may go unnoticed until massive bleeding occurs. Patients often complain of weakness, fatigue, shortness of breath, and painless anal bleeding.
2.6 Diverticular Disease
Diverticula are small pouches in the colon wall, usually found at weak points where blood vessels pass through the muscle layer. Over time, these blood vessels harden and become prone to rupture, leading to bleeding.
2.7 Colon and Rectal Tumors
Both benign and malignant tumors frequently develop in the colon and rectum. People over 50 are most commonly affected, but tumors can also occur in younger individuals.
When tumors bleed, it is typically slow, chronic, and occurs in small amounts. As cancer progresses, additional symptoms may appear, including weight loss, changes in stool size and consistency, a feeling of rectal fullness, or constipation. A definitive diagnosis requires a colonoscopy with a biopsy.
2.8 Upper Gastrointestinal Bleeding
Another common source of anal bleeding is upper gastrointestinal (GI) bleeding, usually from the stomach or duodenum. This often presents as black, tarry stools (melena). However, if the bleeding is severe, it can result in bright red blood in the stool.

3. What is the Medical Treatment for Rectal Bleeding?
The treatment for rectal bleeding depends on its cause and source. Regardless of the location of the bleeding, if a patient has significant blood loss, treatment will begin with stabilizing their condition. Hospitalization is required if the bleeding does not stop or if the patient’s vital signs are abnormal.
Other treatment options will depend on the suspected cause of the bleeding. A gastrointestinal surgeon, gastroenterologist, or ulcerative colitis specialist may be involved in the treatment plan.
4. Home Remedies for Rectal Bleeding
If rectal bleeding is minor and identified as being caused by hemorrhoids or anal fissures, home treatment is often considered by doctors.
Home treatment may include using ointments and suppositories. These over-the-counter medications can be purchased without a prescription. However, if symptoms do not improve within a week of treatment or if the person is over 40 years old, they should consult a doctor for further evaluation.
Simple home care methods for rectal bleeding include:
- Drinking 8-10 glasses of water daily.
- Bathing daily to keep the skin around the anus clean.
- Increasing fiber intake in the diet.
- Avoiding prolonged straining during bowel movements.
- Taking sitz baths (warm water baths covering the hips and buttocks), which may help relieve itching, pain, and discomfort from hemorrhoids.
- Limiting alcohol consumption, as alcohol contributes to dehydration, which can lead to constipation.
Rectal bleeding may indicate a gastrointestinal disorder or specific anorectal conditions such as hemorrhoids, anal fissures, or anorectal malignancies. Depending on the cause, rectal bleeding may or may not be accompanied by pain. If the condition is caused by dietary habits and lifestyle factors leading to constipation, medical intervention may not be necessary. However, if rectal bleeding is associated with serious complications, the patient should visit a healthcare center for examination and treatment.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.