This is an automatically translated article.
The article was written by Specialist Doctor I Nguyen Thi Minh Thuyen - Pathologist, Laboratory Department - Vinmec Danang International General Hospital.Many cases of thyroid cancer are detected early. Today, most thyroid cancers are detected much earlier than in the past and can be treated successfully.
A. Can thyroid cancer be detected early?
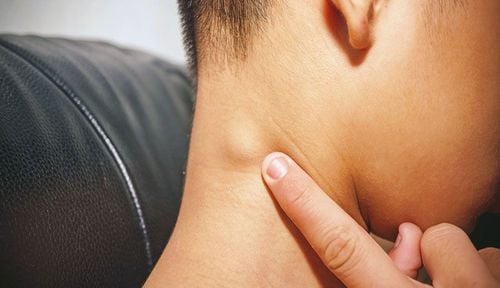
Most thyroid cancers are found early when a patient comes to the doctor because they notice lumps or nodules in the neck. If you have symptoms such as a large mass or swelling in your neck, you should see your doctor right away. Early detection of thyroid cancer during routine health check-ups. Sometimes thyroid cancer is found early with imaging tests, like an ultrasound or CT scan, for other health problems. Blood tests or thyroid ultrasound can detect changes in the thyroid gland, but these tests are not recommended for screening for thyroid cancer except in people at high risk, such as a family history. family with thyroid cancer.People with a family history of medullary thyroid cancer (MTC), with or without multiple endocrine neoplasia type 2 (MEN 2), may be at very high risk of developing the cancer. These people should get genetic testing at a young age to see if they carry the genetic variations associated with MTC. For people who may be at risk but aren't getting genetic testing, blood tests and thyroid ultrasounds can help find MTC at an early stage, when it's still curable.

Hầu hết các ung thư tuyến giáp được phát hiện sớm khi bệnh nhân đến khám vì nhận thấy các khối u hoặc nốt ở cổ
B. Diagnosis of Thyroid Cancer
1. Signs and symptoms of thyroid cancer Thyroid cancer can cause any of the following signs or symptoms:A lump in the neck, which sometimes grows quickly Swelling in the neck Pain in the front neck, sometimes spreading to the ears Hoarseness or voice change that doesn't go away Difficulty swallowing Difficulty breathing Persistent cough that isn't caused by a cold If you have any of these signs or symptoms, see your doctor right away. These symptoms may not be due to cancer or even other cancers in the neck area. Tumors in the thyroid gland are more common and are usually benign. However, if you have any of these symptoms, it's important to see your doctor to find out the cause and get treatment, if needed.
2. Medical history and physical exam If there are any signs or symptoms that suggest you may have thyroid cancer, your doctor will want to know your complete medical history. You will be asked questions about your risk factors, possible symptoms, and any other health problems or concerns. If someone in your family has had thyroid cancer (especially medullary thyroid cancer) or adrenal medulloblastoma (pheochromocytomas), tell your doctor, as you may be at higher risk of developing this condition.
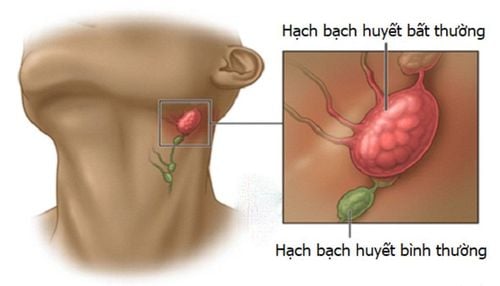
Your doctor will check to get more information about signs of thyroid cancer and other health problems, paying particular attention to the size and density of your thyroid gland and any lymph nodes in your neck. friend.

Khó nuốt, khó thở có thể là biểu hiện của ung thư tuyến giáp
Find suspected areas of possible cancer See how far the cancer may have spread Determine the effectiveness of treatment ● Ultrasound
Ultrasound uses sound waves to create images of parts of your body that are not exposed to radiation. Ultrasound helps:
Determine if nodules are solid or contain fluid (solid nodules are more likely to be cancerous) Check the number and size of thyroid nodules See if there are any metastases in nearby lymph nodes due to cancer thyroid cancer or not. Guide the biopsy needle to the nucleus to collect samples ● Iodine scan (radioiodone scan)
Scans help determine: A tumor in the neck could be thyroid cancer. Helps determine if diagnosed differentiated thyroid cancers (papillary, follicular or Hürthle cell) have spread. Medullary thyroid cancer cells do not absorb iodine, so scintigraphy is not used for this cancer. With this test, a small amount of radioactive iodine (I-131) is taken by mouth (pill) or intravenously. The iodine is then absorbed by the thyroid gland (or thyroid cells anywhere in the body). A special camera is used a few hours later to view the location and measure the amount of radioactive activity. Cold nodule: The abnormal area of the thyroid gland is less radioactive than the surrounding tissue. Cold nodules can be benign or cancerous Hot nodules: areas with more radiation, usually not cancerous. Therefore, this test cannot diagnose thyroid cancer
After surgery for thyroid cancer, whole-body 5 scans help look for the possibility of cancer spreading throughout the body. Postoperative scintigraphy is even more sensitive if the thyroid is completely removed because radioactive iodine is absorbed by any remaining thyroid cancer cells.
Because any type of iodine in the body can interfere with this test, foods or medicines containing iodine should be avoided for a few days before the scan.

Xạ hình giúp xác định khối u ở cổ có phải là u tuyến giáp hay không
If you've been diagnosed with thyroid cancer (especially follicular thyroid carcinoma), you may have a chest X-ray to see if the cancer has spread to the lungs.
● Computed tomography (CT) scan
CT scans produce detailed cross-sectional images of the organs. CT can help determine the location and size of thyroid cancers and whether they have spread to nearby areas or to the lungs.
● Magnetic resonance imaging (MRI)
MRI uses a magnetic field instead of radiation like CT does. An MRI can detect thyroid cancer or cancer that has spread to nearby or distant organs.
● A positron emission tomography (PET) scan
PET can show which organs the cancer has spread to.
3.2. Blood tests A blood test does not identify thyroid cancer, but helps to determine if the thyroid gland is functioning normally, so that other tests can be ordered. They can also be used to monitor certain cancers.
Thyroid stimulating hormone (TSH)
Blood tests of thyroid stimulating hormone (TSH or thyrotropin) may be used to check the general functioning of the thyroid gland. TSH levels, which are made by the pituitary gland, can be high if the thyroid is not producing enough hormone. This mechanism helps to select imaging tests (such as ultrasound or scintigraphy) to evaluate a thyroid nodule.
In thyroid cancer, TSH levels are usually normal.

Xét nghiệm máu không xác định được ung thư tuyến giáp, nhưng giúp biết được chức năng tuyến giáp hoạt động có bình thường không
These are the main hormones produced by the thyroid gland. Levels of these hormones also help assess thyroid function.
T3 and T4 levels are usually normal in thyroid cancer.
●Thyroglobulin
Thyroglobulin is a protein produced by the thyroid gland. Blood levels of thyroglobulin cannot be used to diagnose thyroid cancer, but are necessary after treatment. The current conventional treatment for thyroid cancer is to remove most of the thyroid gland, followed by radioactive iodine treatment to destroy any remaining thyroid cells.
This treatment will cause blood thyroglobulin levels to drop sharply within a few weeks. If thyroglobulin is not low, this means that thyroid cancer cells may remain in the body. If thyroglobulin levels rise again after falling low, it is a sign that the cancer may have returned.
● Calcitonin
Calcitonin is a hormone that helps regulate calcium. It is made by C cells, the source of medullary thyroid cancer (MTC). If MTC is suspected or if you have a family history of the disease, a blood calcitonin test may be suggestive of the diagnosis of MTC. This test is also indicated to see the possibility of MTC recurrence after treatment.
● Carcinoembryonic antigen (CEA)
Patients with medullary thyroid carcinoma (MTC) often have high blood levels of CEA. CEA can help monitor this type of cancer.
●Other blood tests
If surgery is scheduled, you will have tests to check your blood cell count, blood clotting function, and liver and kidney function tests.
Medullary thyroid carcinoma (MTC) can be caused by an inherited syndrome that can also cause adrenal myeloma (called pheochromocytoma). Pheochromocytoma can cause problems during surgery when the patient is under anesthesia. This is why patients with MTC who plan to have surgery are often screened to see if they have pheochromocytoma. Therefore, a blood test for epinephrine (adrenaline) and/or a urine test for its breakdown products (metanephrine) is required.
3.3. Examination of the vocal cords (laryngoscopy) Thyroid tumors can sometimes affect the vocal cords. If you're having surgery for thyroid cancer, you may need a laryngoscopy first to see if your vocal cords are working properly.
3.4. Pathological tests The definitive diagnosis of thyroid cancer must be based on pathological tests.
● Fine needle aspiration (FNA)
The simplest way to evaluate a thyroid mass for benign or cancerous nodules.

Chọc hút bằng kim nhỏ là cách đơn giản nhất để đánh giá một khối tuyến giáp là nhân lành tính hoặc ung thư
Then the patient samples are sent to the Pathology laboratory, to analyze whether the cells are cancerous or benign.
Fine-needle aspiration is usually performed on all thyroid nodules large enough to be palpated. But doctors often use ultrasound-guided sampling to collect samples, especially small, deep-seated nodules, helping to ensure that the sample is in the correct position. FNA is also indicated to take cells from the lymph nodes in the neck to see if they have metastasized.
Occasionally, the FNA will need to be repeated because the samples do not contain enough cells for diagnosis. If the test result is “suspected” or “of undetermined significance”, it means that the result is uncertain whether the thyroid nodule is benign or malignant.
●biopsy
If the diagnosis is not clear after FNA, you may need a biopsy to get a better sample, especially if your doctor has reason to think the thyroid nodule could be cancerous.
These biopsies can be:
Frozen section: remove the thyroid nodule or thyroid lobe in the operating room, then send fresh thyroid tissue to the pathology laboratory, the technician will handle it. and thinly cut the thyroid tissue at - 20 degrees Celsius, stain the specimen and the pathologist reads the diagnostic results under the microscope, the thyroid nodules are benign or malignant, notify by phone to the operating room for the surgeon to operate. treatment for the next steps. This test takes 30-45 minutes to perform. Core biopsy: Using a larger needle, removing the cores of thyroid tissue for histopathology, usually results in 3-5 days. Open biopsies : including thyroidectomy, lobectomy, and complete thyroidectomy 3.5. Molecular testing In some cases, doctors may order molecular tests to look for specific genetic changes in cancer cells. This can be done for different reasons:
If the FNA results are not clear, your doctor may order more testing to see if there is a BRAF or RET/PTC genetic variation. Identifying one of these changes increases the likelihood of thyroid cancer. For some types of thyroid cancer, molecular tests can identify changes in certain genes (such as the BRAF, RET/PTC, or NTRK gene), and can help with treatment. targeted drugs. When we notice abnormalities in the body, we need to go to the doctor immediately, have a general examination as well as a specialist to detect the disease as soon as possible. Doctors recommend that we go for a regular check-up once a year to understand our health status, as well as have a direction to screen for early treatment.
Please dial HOTLINE for more information or register for an appointment HERE. Download MyVinmec app to make appointments faster and to manage your bookings easily.
Article referenced source: American Cancer Society