The HCV RNA test helps identify the hepatitis C virus in the body. Currently, researchers have not been able to observe this virus under an electron microscope or cultivate it in laboratory environments. However, they have identified the HCV genome, allowing them to infer the virus’s basic structure. Proper interpretation of quantitative hepatitis C virus test results is crucial for determining viral load.
This article was written under the professional guidance of doctors from the Department of Gastroenterology - Hepatology, Vinmec International General Hospital.
1. What is Hepatitis C?
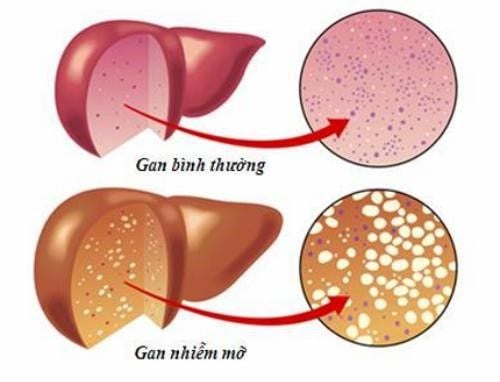
Hepatitis C is a liver infection caused by the presence of the hepatitis C virus (HCV), which can lead to liver cell inflammation, impaired liver function, and permanent damage. This disease can progress to serious complications such as cirrhosis and liver cancer.
Hepatitis C manifests in two main forms: acute and chronic. Acute hepatitis C typically lasts around six months, and in some cases, the infection may resolve on its own without treatment. However, not all cases are so fortunate, as the disease can progress to the chronic stage. Chronic hepatitis C occurs when the virus persists in the body for more than six months. At this stage, the infection cannot be completely cured and may lead to severe complications such as cirrhosis, liver cancer, or even life-threatening conditions.
Since hepatitis C often presents no clear symptoms in its early stages, early detection is challenging. The HCV RNA test is currently the most effective diagnostic method, allowing for the detection of the virus in the blood even before clinical symptoms appear.
2. What is the HCV RNA Test and How is it Performed?
The HCV RNA test is a molecular biology test used to detect the presence of HCV RNA and determine the viral load in the blood. This test utilizes PCR (Polymerase Chain Reaction), a technique that amplifies DNA in a test tube through multiple temperature cycles.
During the HCV RNA test, the serum or plasma from a patient’s blood sample is separated. The RNA of the hepatitis C virus present in this sample is then extracted and placed into a test tube. In the test tube, the viral RNA undergoes reverse transcription to produce complementary DNA (cDNA). This cDNA is then amplified into billions of copies, enabling the detection of the virus. Thanks to its ability to amplify even a minuscule amount of RNA, the HCV RNA test is highly sensitive and can detect the virus even at very low concentrations.
Additionally, by applying quantitative PCR (qPCR), also known as real-time PCR, doctors can precisely determine the initial viral load in the sample. In principle, qPCR operates similarly to traditional PCR but includes the added capability of quantifying the original viral load. This is achieved through an optical detection system that monitors the reactions occurring in the test tube during amplification.
The HCV RNA test can be conducted using manually prepared reagents rather than pre-packaged commercial test kits, making it an entirely open technique. However, to ensure the accuracy of results, it is crucial for the test operator to include proper control samples to identify and eliminate potential errors during the testing process.
So, how should the quantitative results of the hepatitis C virus test be interpreted?

3. How to Interpret the Hepatitis C Viral Load Test Results
When receiving HCV RNA test results, how can one interpret the quantitative viral load? For example:
- What do "below the detection limit" and "not detected" results mean?
If the HCV RNA test result states "below the detection limit," it indicates that the hepatitis C virus may no longer be present in the patient’s blood, or there may still be a very small amount of the virus that is too low for the test to detect. This does not completely confirm that the virus has been entirely eliminated from the patient’s body.
According to the interpretation of the hepatitis C viral load test results, if the test result states "not detected" or "Target Not Detected," it means that no hepatitis C virus has been found in the patient's blood. This is the ideal outcome that every hepatitis C patient hopes for, as it indicates that the virus has been completely eliminated from the body.
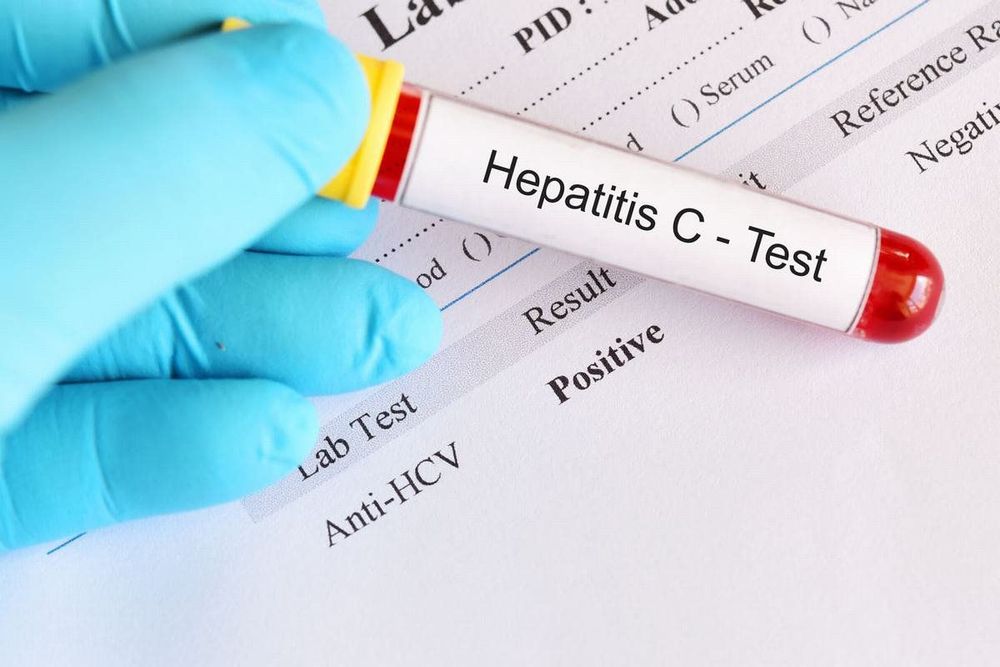
If a patient undergoes testing with a machine that has a low detection threshold after four weeks of antiviral treatment and receives a result of "not detected," it indicates a high likelihood that the patient has completely recovered.
4. Does a Positive HCV RNA Test Result Require Specific Treatment?
Hepatitis C often presents no symptoms or only vague, nonspecific ones. However, the virus silently invades and replicates within liver cells. If this condition persists for years, it can severely damage liver cells, leading to complications such as chronic hepatitis, cirrhosis, and even liver cancer. Individuals infected with hepatitis C have a high risk—ranging from 17% to 20%—of developing chronic hepatitis and other serious complications.
This differs from hepatitis B, where only chronic hepatitis B patients (those with elevated ALT levels or liver damage detected through biopsy or FibroScan) require specific treatment.
Therefore, as soon as a positive HCV RNA test confirms a hepatitis C infection, the patient should immediately receive specific treatment. Waiting for ALT levels to rise significantly or for imaging tests to detect liver damage is no longer a prerequisite for starting treatment.
Before beginning treatment, patients must undergo two essential tests: an HCV RNA quantitative test and an HCV genotype test. These tests help doctors monitor treatment effectiveness, develop a suitable treatment plan, and determine the appropriate treatment duration for each case. After three months of treatment, patients will undergo another HCV RNA quantitative test to assess the therapy’s effectiveness.
- If the hepatitis C viral load does not decrease or decreases by less than 100-fold, the doctor will consider changing the treatment approach due to poor response.
- If the viral load decreases by more than 100-fold, the treatment regimen is deemed effective. The doctor will decide on the duration of continued treatment based on the patient’s HCV genotype. For example, if a patient is infected with HCV genotype 1, treatment may need to be extended by an additional nine months, totaling 12 months. For other genotypes, such as 2 or 6, the additional treatment duration is three months, making the total treatment period six months.
Before concluding treatment, doctors will require another HCV RNA test to confirm whether the virus remains in the bloodstream. If the result is still positive, treatment should continue for another three months until a negative result is achieved.
After completing treatment, regular follow-up with HCV RNA testing every three months is necessary to monitor for recurrence or reinfection. If the test result ever turns positive again, it indicates relapse or reinfection, requiring the patient to resume the initial treatment plan.
5. What Does a Positive Anti-HCV Blood Test Mean?
Anti-HCV is a specific antibody against the hepatitis C virus (HCV). A positive anti-HCV blood test result indicates that the patient’s blood contains antibodies against HCV. This could mean the patient is currently infected or was previously infected but has since recovered.
However, the presence of anti-HCV antibodies does not guarantee that the body has developed sufficient protective immunity to completely eliminate the virus. In most cases, the immune system cannot mount a strong enough response to effectively combat an HCV infection.
Only a small percentage of patients recover due to the body's nonspecific immune defenses against HCV. In most cases, the virus remains in the body, continues to replicate in liver cells, and releases new viral particles into the bloodstream.
To accurately determine whether a patient is infected with the hepatitis C virus (HCV), doctors need to order an HCV RNA test—a specialized test that detects the viral nucleic acid in the blood. If the HCV RNA test result is positive, it confirms that the hepatitis C virus is still present in the blood and that the patient is actively infected with HCV.
6. How Long After HCV Exposure Does the Anti-HCV Test Become Positive?
Typically, around 70% of patients will start producing anti-HCV antibodies when they first show symptoms. However, within three months of exposure, this rate can increase to approximately 90%.
One key concern is that most people infected with hepatitis C do not exhibit clear symptoms, leading to a lack of awareness about the importance of early screening.
7. What Should Be Done After a Positive Anti-HCV Test?
When a blood test for anti-HCV returns positive, the next important step is to measure liver enzymes, particularly ALT levels. Elevated ALT levels indicate ongoing liver inflammation. Therefore, additional tests are needed to assess the severity of hepatitis and determine whether specific treatment for chronic hepatitis C is necessary.
8. Can the Anti-HCV Test Yield a False Positive Result?
A false positive occurs when a test incorrectly indicates infection in a person who is not actually infected. This can happen in some cases, particularly in individuals at low risk of hepatitis C, such as blood donors who have minimal risk factors.
For this reason, when an anti-HCV test is positive, doctors typically order additional tests to confirm the result. In clinical practice, most reported false positives turn out to be negative upon further testing.
9. Should Pregnant Women Undergo Routine Anti-HCV Testing?
Routine anti-HCV testing for pregnant women is not widely recommended, as pregnancy does not increase the risk of HCV infection. However, if a pregnant woman falls into a high-risk category—such as those with a history of sharing needles or other risk factors—anti-HCV testing may be considered.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.