Pimples in the ear, similar to those on other parts of the body, develop due to the presence of sebaceous glands and hair follicles in the skin of the outer ear and ear canal. When dirt and bacteria accumulate, they can lead to ear pimples. Are ear pimples harmful, and how should they be safely treated?
Acne consists of various types, including whiteheads, blackheads, pimples, cystic acne, and nodules. It can develop anywhere on the body, especially in areas rich in sebaceous glands, such as the face and back. Acne can also occur in the ear, commonly appearing on the outer ear (auricle) or inside the ear canal.
1. What causes acne in the ear?
Similar to other areas of the skin, the outer ear has sebaceous glands, while the ear canal contains hair follicles and sebaceous secretions. Excessive oil production can contribute to the development of acne.
Additionally, ear acne can result from bacterial growth or the accumulation of dead skin cells in clogged pores. The main causes of bacterial and sebum buildup in the ear, leading to acne, include:
- Inserting fingers or unsterilized objects into the ear
- Wearing dirty earphones without proper hygiene
- Exposure to polluted or dusty environments
- Frequent water retention inside the ear
- Hormonal changes during puberty, pregnancy, or stress-induced imbalance
- Allergic reactions from cosmetics or infections from ear piercings
- Prolonged helmet or hat use, leading to bacterial buildup
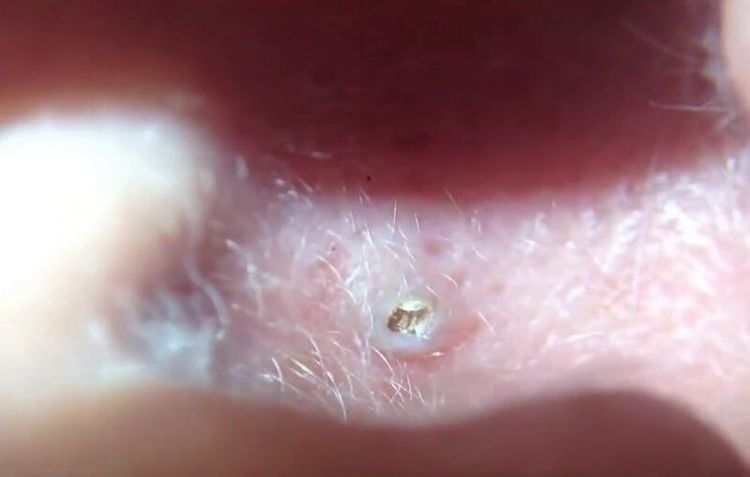
2. Are ear acne dangerous?
Ear pimples can cause significant discomfort and pain. If left untreated, they may lead to complications such as infections, irritation of the ear skin, and the formation of nodules or cysts within the ear. When a pimple in the ear becomes swollen and painful, it may indicate other conditions that are often mistaken for ear acne, such as:
- Granulomas: Soft, reddish skin lesions that may develop due to prolonged pressure, such as from eyeglasses.
- Keloid scars: Raised, red or purple scars caused by excessive collagen production, often accompanied by small birthmarks.
- Seborrheic keratosis: Thickened, flat, light brown skin lesions that form due to excess sebaceous gland activity.
- Epidermoid cysts: Small, slow-growing, subcutaneous lumps that are frequently mistaken for sebaceous cysts.
- Basal cell carcinoma: A type of skin cancer that can sometimes be mistaken for acne.
If an ear pimple becomes swollen, painful, or persists, patients should seek evaluation by a dermatologist for timely treatment.
3. Treatment for ear acne
A common habit among many individuals is squeezing acne, including those inside the ear. Although this method may seem effective for rapid removal, it can also worsen the condition by pushing bacteria and pus (if present) deeper into the pores, leading to skin irritation, scabbing, and scarring. In more severe cases, this may lead to secondary infection and abscess formation, requiring medical treatment.
To prevent the complications mentioned above, it is important to treat ear acne:
- Apply a warm compress (using a heating pad or warm gauze) to reduce inflammation and minimize skin irritation in the ear area. Additionally, this method softens the pimple and helps the pus drain more easily, a technique that is often overlooked.
- Clean the affected area properly: If the pimple ruptures, use a sterile cotton pad soaked in an antiseptic solution, such as povidone-iodine or alcohol, to cleanse the area and prevent infection.
If home treatments for ear pimples prove ineffective, consulting a dermatologist is necessary to determine the exact nature and severity of the condition. Based on this assessment, the doctor may prescribe appropriate acne treatments to prevent scarring.
For mild to moderate acne, treatment may include topical medications such as tretinoin, benzoyl peroxide, or topical antibiotics to control bacterial infection. Additionally, hydrogen peroxide may be prescribed for wound disinfection, alongside pain relievers and non-steroidal anti-inflammatory drugs (NSAIDs) to alleviate discomfort. In cases involving pustules, the physician may perform an incision and drainage procedure to remove accumulated pus.
4. Prevention of acne in the ear
Ear acne can be prevented by maintaining ear hygiene. Practices include:
- Cleaning the ears with clean water or saline solution to remove excess oil and dead skin cells from the outer ear and ear canal.
- Keeping the ears free from dirt and foreign particles to avoid infections.
- Cleaning earphones regularly and minimizing their use when unnecessary.
- Avoiding exposure to polluted or dirty water.
- Allowing air circulation in the ears by limiting the use of tight-fitting headgear or helmets for extended periods.
Patients should seek medical evaluation if they experience:
- Recurrent or persistent ear pimples
- Significant swelling and pain within the ear
- Ear pain accompanied by nausea or fever
While ear pimples are generally not dangerous, they can cause discomfort. Home management includes warm compresses and antiseptic application. However, persistent or recurrent cases that interfere with daily life should be evaluated by a dermatologist.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.