This article has been medically reviewed by Dong Xuan Ha, Specialist Level I, Deputy Head of the Department of General Examination & Internal Medicine at Vinmec Ha Long International General Hospital
Gastric mucositis is one of the most common gastrointestinal conditions today. In some cases, it can lead to ulcers and increase the risk of stomach cancer. However, with proper treatment, gastric mucositis often improves quickly.
1. What is Gastric Mucositis?
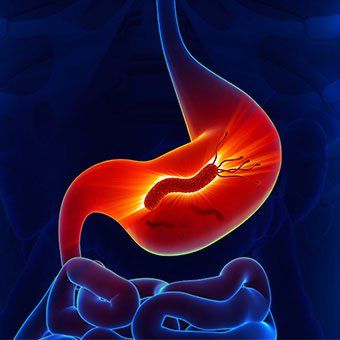
Gastric mucositis is a condition in which the stomach lining (also known as the gastric mucosa) becomes inflamed, irritated, and eroded due to damage. The primary causes often include bacterial infections, excessive use of pain relievers, or other related factors.
This condition can develop suddenly or progress gradually over time. In most cases, gastric mucositis can improve quickly with proper treatment. However, in some instances, it may lead to ulcers and increase the risk of stomach cancer if left untreated.
1.1 Acute Gastric Mucositis
This condition occurs when the stomach lining suddenly becomes inflamed or swollen, causing severe pain and discomfort. Acute gastritis can be triggered by various factors, including injury, stress, stimulants, NSAIDs, spicy foods, or infections caused by bacteria and viruses. The pain is typically temporary and lasts for a short period.
1.2 Chronic Gastric Mucositis
Chronic gastritis involves long-term inflammation and damage to the stomach lining, although the symptoms may be mild. Over time, the gastric mucosa gradually thins as immune system responses, including lymphocytes, destroy stomach cells.
If chronic gastritis persists for many years, it can progress to mucosal atrophy, significantly increasing the risk of stomach cancer.
2. Causes of Gastric Mucositis
Gastric mucositis occurs when the protective barrier of the stomach lining becomes weakened or damaged, allowing digestive fluids to irritate and erode the mucosa. Some of the main causes include:
2.1 Bacterial Infection
Helicobacter pylori (H. pylori) infection is one of the most common bacterial infections, affecting approximately 50-70% of the global population. However, only a small percentage of infected individuals develop gastritis or other digestive issues.
H. pylori infection can result from genetic factors, lifestyle habits, or dietary choices.
2.2 Frequent Use of Pain Relievers
Excessive or prolonged use of pain relievers and nonsteroidal anti-inflammatory drugs (NSAIDs) can lead to both acute and chronic gastritis by weakening the stomach’s protective lining, making it more susceptible to damage.
2.3 Aging
Older adults are at higher risk of developing gastric mucositis compared to younger individuals. This is due to an increased likelihood of H. pylori infection, weakened immune function, and faster mucosal erosion as the body ages.
2.4 Alcohol Abuse
Excessive alcohol consumption can irritate and damage the stomach lining, making it more vulnerable to digestive acids, which can contribute to acute gastritis.

2.5 Stress
Psychological instability and chronic stress can contribute to gastric mucositis, particularly in cases involving post-traumatic stress, infections, or surgery. High-stress levels can exacerbate symptoms and complicate the condition.
2.6 Cancer Treatments
During cancer treatment, patients undergoing chemotherapy or radiation therapy may experience gastritis as a side effect
2.7 Autoimmune Gastritis
Autoimmune gastritis occurs when the body’s immune system mistakenly attacks the stomach lining, leading to damage and erosion of its protective barrier. This condition is more common in individuals with autoimmune disorders, such as Hashimoto’s thyroiditis and type 1 diabetes. Additionally, vitamin B12 deficiency is often associated with autoimmune gastritis, as it can impair the stomach's ability to produce intrinsic factor, a protein necessary for B12 absorption.
3. Prolonged Stomach Pain and Associated Symptoms of Gastric Ulcers
The stomach is a crucial part of the digestive system, acting as a food reservoir and connecting to the duodenum. A normal stomach can hold approximately 1 - 1.5 liters of food and liquid.
The primary functions of the stomach include motility, peristalsis, secretion, and digestion, which rely on muscular contractions, hydrochloric acid, and digestive enzymes. When the stomach is full, its muscle tone decreases; when it is empty, the muscle tone increases.
Each day, the stomach secretes around 1.5 liters of gastric juice, containing proteins, albumin, immunoglobulins, amino acids, and digestive enzymes such as pepsinogen, pepsin, glucids, and glycoproteins.
The stomach consists of five layers, with the mucosa as the outermost layer, which contains the gastric glands. The mucosa plays a vital role in protecting the stomach from harmful agents.
However, this mucosal layer is fragile and can be easily damaged by various factors. When inflamed, it thins out, making the stomach vulnerable to ulcers. If left untreated, gastric mucositis can lead to serious complications, such as:
- Peptic ulcers: One of the most common causes of stomach pain, often accompanied by acid reflux, bloating, belching, and epigastric pain. Gastric ulcers are becoming increasingly common.
- Gastrointestinal bleeding
- Stomach perforation.
- Pyloric stenosis
- The formation of tumors in the stomach increases the risk of stomach cancer.
Some individuals with gastric mucositis may not exhibit any noticeable symptoms. However, common signs include:
- Black stools, possibly with a tar-like consistency.
- Nausea.
- Recurring abdominal pain.
- Bloating and stomach distension.
- Indigestion and difficulty digesting food.
- Burning sensation in the stomach, especially between meals or at night.
- Frequent hiccups.
- Loss of appetite.
- Vomiting blood or substances that resemble coffee grounds.
4. Mechanism of Gastric Ulcer Development
The development of peptic ulcers is primarily the result of an imbalance between harmful factors and protective factors in the stomach lining.
Pathogenic factors are often attributed to the excessive secretion of hydrochloric acid (HCl) and/or pepsin in gastric juice, infection with Helicobacter pylori (HP), excessive use of anti-inflammatory drugs, high alcohol consumption, and smoking.
Additionally, protective factors that safeguard the gastric mucosa from damage include mucin, bicarbonate, the capillary network, and, most importantly, the integrity of the gastric epithelial cell layer.
5. Principles of Gastric Mucosal Healing
Based on the pathogenesis, the recovery process of the gastric mucosa in cases of inflammation or ulceration must adhere to the following fundamental principles:
- Reducing gastric acid and pepsin secretion using mucosal-healing medications, such as acid secretion inhibitors or neutralizing agents.
- Enhancing mucosal protective factors through drugs that form a protective barrier or promote ulcer healing. These agents help minimize the impact of ulcerogenic factors and create favorable conditions for mucosal regeneration over time. Additionally, mucosal-healing drugs can inhibit HP (a major cause of gastric ulceration)
- Promoting epithelial cell regeneration, mucous secretion, and prostaglandin production through appropriate therapeutic interventions.
- Eradicating Helicobacter pylori using antibiotic regimens or other supportive medications.
- Implementing supportive treatments and improving overall health to facilitate gastric mucosal recovery.
6. Methods for Healing Gastric Mucosal Inflammation in Patients with Gastric Ulcers
6.1 Medication Use
Currently, medication is the primary approach for treating gastric ulcers. However, before initiating treatment, patients must consult a physician to confirm the presence of gastric ulcers.
To achieve optimal therapeutic outcomes, patients should strictly adhere to medical guidelines, avoiding self-medication or altering prescribed treatments without professional consultation.
Commonly used drugs for gastric mucosal healing in ulcer treatment include:
- Gastric acid secretion inhibitors
- Gastric acid neutralizers
- Antibiotics effective against HP
- Mucosal-healing agents, create a protective barrier to shield ulcerated areas from harmful factors.
6.2 Follow-up Visits with a Specialist
Gastric ulcer medications are typically prescribed for 2 to 4 weeks, depending on the patient's condition and individual response to treatment.
Follow-up examinations after completing a treatment course are crucial for doctors to assess the healing progress and determine whether any adverse drug reactions have occurred.
Some patients, after experiencing symptom relief, may discontinue or alter their medication regimen without consulting a physician, skip follow-up visits, or even use prescriptions from others. These actions can worsen the condition and negatively impact overall health.
Regular follow-up visits remain necessary to prevent recurrence even when the ulcers have stabilized.
6.3 Dietary Support for Gastric Mucosal Healing
Certain foods have been found to aid in gastric mucosal recovery effectively, yet they are not widely recognized. These include:
- Aloe Vera: Aloe vera juice not only promotes skin health but also helps alleviate bloating caused by ulcers. Additionally, it has mild laxative properties and supports digestion.
- Yellow Turmeric: A combination of turmeric powder and honey exhibits anti-inflammatory effects, prevents ulcer formation, and reduces gastric acid secretion.
- Black Turmeric: Consuming black turmeric with warm water can suppress gastric acid secretion and enhance digestive function.
However, natural herbal remedies still carry risks of allergic reactions, side effects, or toxicity. Therefore, it is essential to consult a healthcare professional before use.
6.4 Dietary and Lifestyle Modifications
Individuals suffering from gastric mucosal inflammation often have poor dietary and lifestyle habits, which need to be adjusted as soon as possible to promote healing, reduce ulcer severity, and prevent further complications.
To establish a healthy diet and balanced lifestyle, patients should:
- Limit alcohol consumption, avoid stimulants, and strive to quit smoking.
- Increase intake of fresh vegetables, fruits, and whole grains to support digestion and overall health.
- Ensure adequate sleep by maintaining a regular sleep schedule and avoiding late nights.
- Manage stress levels by staying optimistic and avoiding excessive anxiety.
- Consume soft, easily digestible foods while avoiding acidic, spicy, or overly hot dishes.
- Engage in regular physical activity, such as exercising for at least 30 minutes per day and participating in suitable sports activities.
7. Nutrition for Individuals with Gastric Mucosal Inflammation
7.1 Recommended Foods
Patients should prioritize consuming foods that help control gastric mucosal inflammation and alleviate discomfort. The following are some recommended food categories:
- High-fiber foods: Whole grains, leafy greens, legumes, and fruits.
- Low-fat foods: Fish, vegetables, and lean meats.
- Low-acid foods: Vegetables and legumes.
- Non-carbonated and caffeine-free beverages.
- Probiotic-rich foods: Yogurt, kimchi, and probiotic supplements.
7.2 Foods to Avoid
An unhealthy diet can exacerbate gastric mucosal inflammation. To promote healing, patients should avoid or significantly reduce the consumption of the following:
- Acidic foods such as tomatoes and certain fruits.
- Alcoholic beverages, including beer and liquor.
- Carbonated drinks.
- Coffee.
- High-fat foods.
- Fried foods.
- Fruit juices.
- High-sodium foods.
- Spicy and hot foods.
- Tea.
If any specific food or food group worsens symptoms, patients should immediately discontinue its consumption to prevent further irritation.
There are various methods to promote gastric mucosal healing, but the most crucial factor is strict adherence to medical guidelines, including proper medication use and lifestyle modifications. By taking prescribed medications correctly and maintaining a healthy lifestyle, patients can accelerate gastric recovery and enhance their overall quality of life.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.