Lower back pain is a common symptom associated with menstrual cycle-related conditions, such as premenstrual syndrome (PMS)—a condition that most women experience during their menstrual period. The pain can become more severe in cases of premenstrual dysphoric disorder (PMDD), dysmenorrhea, or endometriosis.
1. Causes of back pain during menstruation
In reality, many factors can contribute to severe lower back pain during menstruation. Several of these causes are linked to underlying gynecological conditions.
1.1. Premenstrual syndrome (PMS)
PMS is a condition that most menstruating individuals experience. Symptoms usually appear about a week before menstruation and subside once the period begins.
Common symptoms of PMS include:
- Breast tenderness;
- Bloating;
- Diarrhea or constipation;
- Abdominal cramps;
- Headaches;
- Mood swings or emotional instability.
For some women, severe lower back pain can be a frequent symptom. This is often related to increased inflammation during menstruation.
Recent research has shown that women with higher levels of inflammation during their menstrual period are more likely to experience severe abdominal cramps and intensified back pain compared to others.
1.2. Premenstrual dysphoric disorder (PMDD)
PMDD is a more severe form of premenstrual syndrome (PMS). This disorder is characterized by intense PMS symptoms that significantly interfere with a woman's daily life, including education, work, and personal relationships.
The most common symptoms of PMDD include:
- Allergic reactions, acne outbreaks, and inflammatory conditions;
- Psychological changes such as anxiety, depression, or severe mood swings;
- Neurological symptoms like heart palpitations and dizziness;
- Digestive issues such as nausea, vomiting, and diarrhea.
Similar to PMS, increased inflammation during PMDD can lead to severe lower back pain. Sometimes, back pain may also be a secondary effect of other PMDD symptoms, such as:
- Vomiting;
- Diarrhea;
- Pelvic pressure.
1.3. Dysmenorrhea (Menstrual Cramps)
Dysmenorrhea is a condition characterized by menstrual cramps that occur during a woman’s period. When experiencing menstrual cramps, the uterus contracts more intensely than usual. This can result in severe cramping, which may sometimes lead to weakness and exhaustion.

When experiencing menstrual cramps, you may encounter the following symptoms:
- Abdominal pain
- Pain radiating down the legs
- Lower back pain
- Diarrhea
- Nausea or vomiting
- Dizziness or headaches
Cramps caused by menstrual pain can spread throughout the lower and upper back. According to a study conducted on 300 women aged 18-25, researchers found that over 84% of them experienced primary dysmenorrhea. Among 261 participants, approximately 16% reported lower back pain symptoms, including: Muscle spasms; Sharp, stabbing pain; Aching discomfort; Intense, sudden pain similar to a stabbing sensation
Primary Dysmenorrhea: Primary dysmenorrhea occurs due to menstrual cramping. Generally, those affected by primary dysmenorrhea experience pain at the start of their period.
During menstruation, the uterus contracts to shed the uterine lining. Prostaglandins, chemical messengers that act like hormones, stimulate the uterus to contract more intensely.
However, if prostaglandin levels are excessively high, the pain becomes more severe. In some cases, these contractions can lead to stomach cramps. Additionally, women may feel pain radiating from the lower back down to the legs.
Secondary Dysmenorrhea: Secondary dysmenorrhea tends to develop later in life. This type of lower back pain during menstruation is caused by an underlying health condition or injury. Generally, prostaglandins still contribute to increased pain intensity in individuals with secondary dysmenorrhea.
1.4. Endometriosis
Endometriosis is a more severe condition affecting women during their menstrual cycle. This disorder is characterized by the displacement of uterine tissue outside the uterus. These misplaced tissues tend to “wander” to other areas of the pelvic region.
Endometriosis can cause:
- Severe abdominal pain
- Dysfunction of various organs
- Scar tissue formation
Common symptoms of endometriosis include:
- Pelvic pain outside of menstruation
- Chronic pelvic pain, especially during and after sexual intercourse
- Prolonged menstrual periods
- Severe menstrual cramps, including lower back pain
In general, lower back pain caused by endometriosis differs from pain associated with PMS, PMDD, and menstrual cramps.
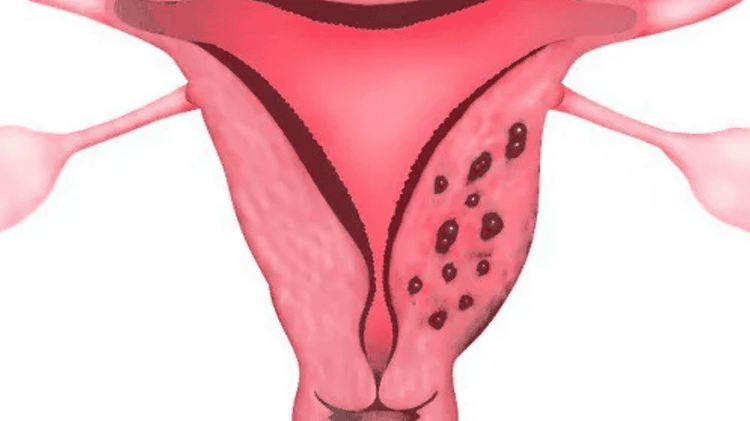
When the endometrial lining moves to other locations outside the uterus, it can cause deep, persistent pain that is difficult to manage using traditional methods such as chiropractic adjustments or massage therapy.
Endometriosis is a serious health condition for women. Therefore, early diagnosis is essential to determine the most appropriate treatment approach for each patient.
1.5. Uterine fibroids
Uterine fibroids are non-cancerous growths that develop in the uterus. This condition can cause intense pain, including lower back pain during menstruation.
In general, these fibroids can sometimes resolve on their own without treatment, even those that cause severe symptoms. However, in certain cases, a doctor may recommend surgery to remove them.
1.6. Other conditions
Several underlying conditions can also affect the abdomen and lower back during menstruation, including:
- Uterine fibroids
- Infections
- Tumors
- Pelvic inflammatory disease (PID): A bacterial infection that typically starts in the uterus and spreads to other areas.
- Other conditions affecting reproductive organs, such as abnormal pregnancy positions, miscarriage, or ectopic pregnancy.
If your lower back pain becomes severe, it is best to consult a doctor for proper diagnosis and treatment.
2. Diagnosing lower back pain during menstruation
To diagnose or determine the cause of lower back pain during your menstrual cycle, you may need to undergo various medical examinations, including:
- Gynecological exam
- MRI scan to obtain detailed images of internal organs
- Ultrasound to assess reproductive organs
- Hysteroscopy: A thin, lighted instrument is inserted through the vagina and into the cervix to examine the inside of the uterus
- Laparoscopy: A thin tube with a lens and light is inserted through the abdominal wall to help doctors detect pelvic and abdominal tumors

3. Treatment methods for lower back pain during menstruation
Currently, medications, complementary therapies, and surgery are the most common treatment methods for severe lower back pain during menstruation.
3.1. Hormonal birth control
This method is often prescribed for menstrual cramps and includes contraceptives that combine estrogen and progesterone. There are also alternative options that contain only progesterone.
Overall, hormonal birth control can significantly reduce pain and discomfort caused by menstruation. Additionally, it helps alleviate the following conditions:
- Premenstrual syndrome (PMS)
- Premenstrual dysphoric disorder (PMDD)
- Endometriosis
- Dysmenorrhea (menstrual cramps)
3.2. Nonsteroidal anti-inflammatory drugs (NSAIDs)
These include ibuprofen, aspirin, and naproxen, which are effective in reducing pain and inflammation.
A recent study found that NSAIDs (such as ibuprofen and naproxen) are more effective in relieving menstrual pain than aspirin.
3.3. Transcutaneous electrical nerve stimulation (TENS)
This technique uses electrodes to deliver mild electric shocks to the skin, stimulating the release of endorphins—the body's natural painkillers.
A study on a 27-year-old female patient showed that combining spinal mobilization, heat therapy, and TENS significantly reduced moderate to severe lower back pain after 3–4 monthly treatment cycles.
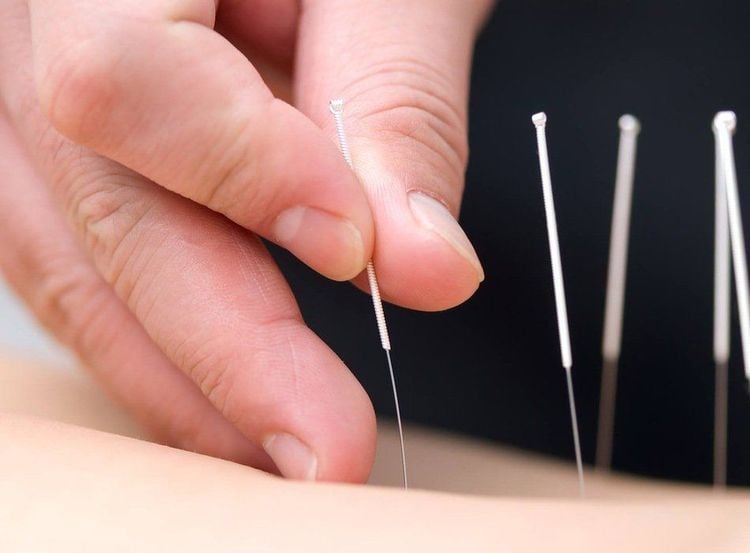
3.4. Acupuncture and acupressure
These complementary therapies focus on applying pressure to various points on the body to relieve pain and promote healing. Research has shown that 12 acupuncture sessions can significantly reduce menstrual pain for up to one year. Additionally, clinical trials have found that acupressure is an effective method for relieving menstrual cramps.
3.5. Surgery
Surgery may be performed in cases of endometriosis, aiming to remove uterine tissues that cause discomfort. In some instances, doctors may recommend removing small portions of displaced uterine tissue.
If the damage and scarring are severe, the patient may require a total hysterectomy, including removal of the uterus, cervix, and ovaries.
4. Home Remedies
Home remedies can effectively help relieve lower back pain during menstruation. Here are some methods you can try:
- Over-the-counter medications: Aspirin, ibuprofen, or pain-relief creams can help ease menstrual cramps. Most pain-relief creams contain capsaicin, a powerful anti-inflammatory compound that provides pain relief. You can apply these creams to massage the lower back and relax the muscles.
- Heat therapy: Apply a warm compress to the lower back to alleviate pain. While doing this, try to relax your back muscles for faster relief.
- Rest and relaxation: Severe lower back pain can interfere with your work. It’s best to set aside adequate rest time for yourself. Try relaxing with music, a book, light yoga, or a warm bath—all of which can stimulate endorphin production, the body's natural painkiller.
5. Lifestyle tips to reduce lower back pain during menstruation
Unhealthy habits such as smoking or alcohol consumption can worsen inflammation. Additionally, excessive intake of caffeine, fats, and salty foods can aggravate menstrual symptoms.
To alleviate PMS symptoms, including lower back pain, try the following: Drink plenty of water; Eat more vegetables and fruits; Consume anti-inflammatory foods.
Regular exercise can also help by stimulating the body's natural endorphin release, which provides pain relief. If lower back pain makes it difficult to exercise, try gentler activities such as swimming or yoga.
Moreover, sexual activity can be an effective pain relief method. Achieving orgasm may help reduce menstrual cramps and lower back pain.

6. When to see a doctor?
You should consider seeing a doctor if:
- Pain-relief medications are ineffective.
- Home remedies do not provide relief.
- You experience additional symptoms, such as bleeding between periods, pelvic pain, or pain during intercourse.
- The pain is severe enough to prevent you from performing daily activities.
- You develop new menstrual pain or notice worsening symptoms over time.
- Your menstrual bleeding is so heavy that you need to change sanitary pads or tampons frequently.
- You experience other back or muscle-related symptoms, such as pain while walking, difficulty lifting objects, or muscle spasms.
Article reference source: healthline.com, medicalnewstoday.com
Read more:
- Is Lower Back and Abdominal Pain After an Abortion a Sign of Retained Placenta?
- Is it normal to have brown discharge and lower back pain 6 weeks after embryo transfer?
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.